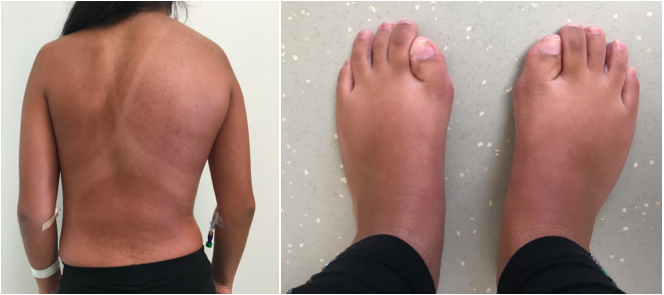
Case Presentation: A 12-year-old female presented to the ER with a 1-week history of painful swelling of her right upper back not alleviated by NSAIDs or warm packs. She denied a history of recent trauma or fever. She has a history of surgical removal of a cranial myofibroma at 5 months of age and persistent swelling of her right quadriceps after routine 6-month vaccination.Physical exam was remarkable for an asymmetric swelling of her right posterior hemi-thorax with loss of landmarks of the right scapula that was mildly tender and firm on palpation. There was no fluctuance, erythema, skin changes, or scoliosis of the spine (Fig.1). Further examination revealed shortened first metatarsals bilaterally (Fig.2) and a palpable mass in the right quadriceps. Chest xray was nonspecific and follow-up ultrasound suggested cellulitis. Baseline labs with uric acid and LDH were normal. MRI was nondiagnostic. Due to concern of malignancy, she underwent US-guided biopsy, which showed nodular fasciitis concerning for early stage fibrodysplasia ossificans progressiva (FOP). After the biopsy, the swelling began to spread across her back. Xrays of the hands, feet, and right femur showed shortened first digits and myositis ossificans of the quadriceps. She was started on high-dose steroids and symptoms improved. Subsequent ACVR1 genetic testing was positive.
Discussion: FOP is a rare, debilitating disorder that can be clinically diagnosed by characteristic congenital malformations of the great toes and progressive heterotopic ossifications throughout childhood. Confirmatory genetic testing reveals a missense mutation causing constitutive activation of the ACVR1 gene promoting bone growth. 87% of patients are initially misdiagnosed, most commonly with cancer. The disease is characterized by episodic flare-ups, often precipitated by trauma, vaccines, or viral infections, consisting of painful soft tissue swellings as skeletal muscle and connective tissue are replaced by bone. Although steroids reduce inflammation in acute flares, there is no cure and on average patients die from thoracic insufficiency in their 4th decade.
Conclusions: Our patient had congenital malformations and a history of prior misdiagnosed FOP flare-ups, but due to the lack of widespread knowledge of FOP, she underwent further harmful testing leading to worsening symptoms and quality of life. Although rare, it is important for hospitalists to be aware of the classic symptoms and exam findings (e.g. great toe abnormalities) associated with FOP to appropriately diagnose the disease early and avoid unnecessary diagnostic procedures.