Background: To curb the growing opioid epidemic, hospitalists need to re-examine inpatient opioid use and increase utilization of alternatives to opioids for pain management. Of 1.1 million nonsurgical inpatients across 286 US hospitals from July 2009 to June 2010, 51% received an opioid during hospitalization and more than half with inpatient exposure were prescribed opioids at discharge. Partnering with The Colorado Hospital Association, we created iALTO (inpatient alternatives to opioids) pain treatment pathways for five common pain types: pleuritic pain, renal colic, extremity pain, acute non-surgical abdominal pain and musculoskeletal pain. The iALTO committee chose these pain types based on electronic health record (EHR) data on the most common pain-related discharge diagnoses. We also used provider surveys and existing literature to determine what pain types would be most suitable for non-opioid therapies.
Methods: This study was conducted on one medical-surgical nursing unit with 22 beds at an academic teaching hospital from August – September 2019. Our target patient population had one of the five pain types listed above. We excluded patients with sickle cell disease or on hospice, and patients on the medical oncology or consult services. Our target providers were hospitalists and inpatient family medicine providers. The intervention group consisted of our target patients on one designated hospital unit who was cared for by our target providers. The non-intervention group was target patients on other hospital nursing units, who were cared for by services other than our target providers. Both nurses and physicians received education about the iALTO pain treatment pathways. The pathways were distributed via email, posted in work areas and available digitally in the EHR, along with pharmacologic guidance and tip sheets for uncommonly used medications. Data was obtained from our EHR. The outcome measure was percent reduction in the average milligram of morphine equivalents per day (MME) per patient between the baseline period (August 2018- March 2019) and the study period. We compared these results to similar data for the non-intervention group. The other outcome measures were patient satisfaction with pain management as determined by nurse surveys and provider attitudes regarding the usefulness of the pathways.
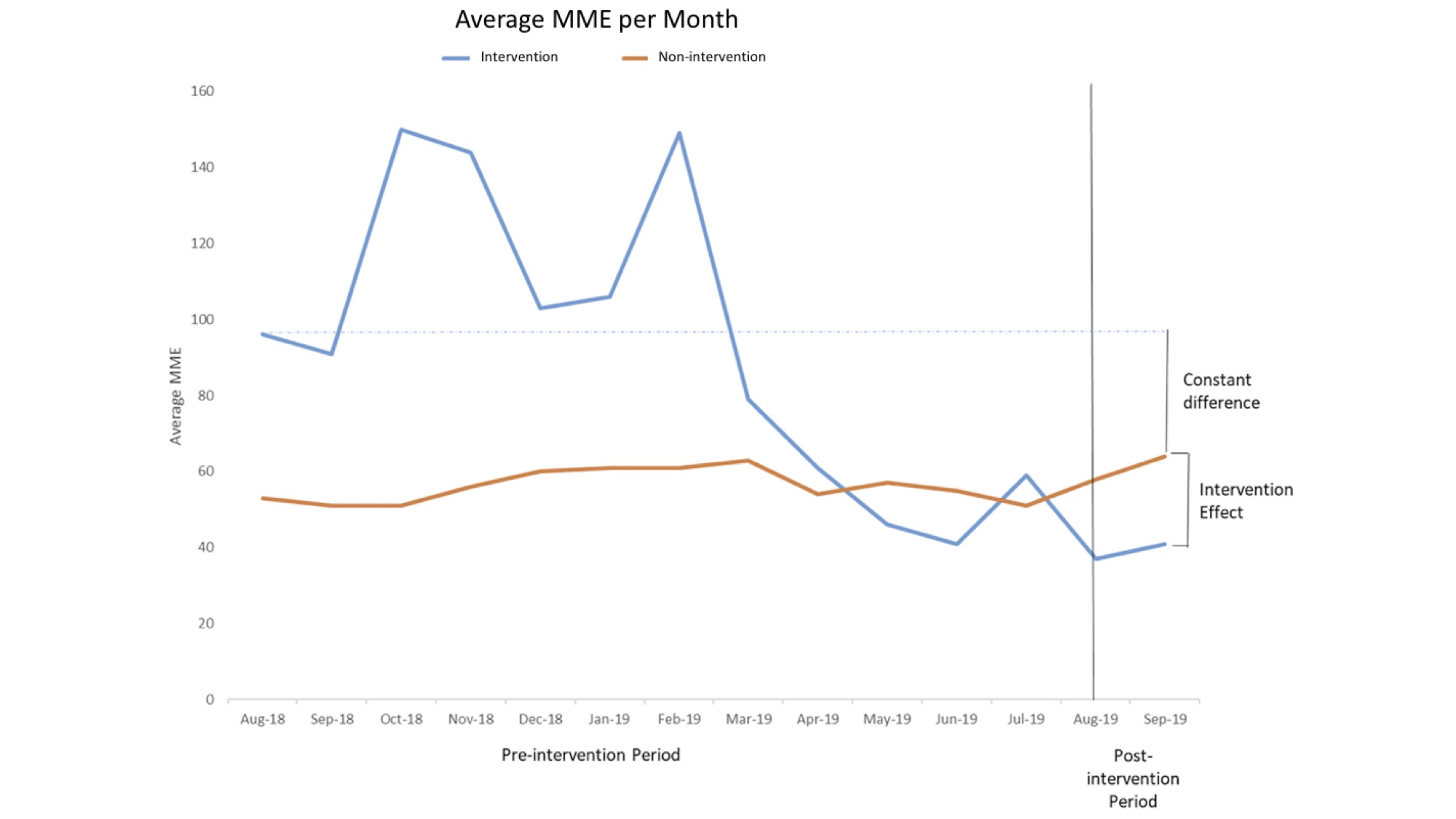
Results: 157 patients were included in the intervention group. For the intervention group, the average MME per patient was 87 during the baseline period and 39.8 during the study period. The percent difference was a decrease of 54.4%. For the non-intervention group, the average MME per patient was 57 during the baseline period and 58.8 during the study period. The percent difference was an increase of 3%. See Figure 1. We surveyed 10 nurses and 10 providers after the study. 100% of nurses reported that patients were equally or more satisfied with their pain management during the study. 90% of providers said the pathways were helpful.
Conclusions: Using iALTO pathways for five common pain types reduced opioid use for inpatients cared for by hospitalist and family medicine providers. There was no change in patient satisfaction with pain treatment as reported by nurse surveys. Such pathways could be adopted by other hospitals or specialties to reduce unnecessary opioid use.