Background: Discharge planning and transition of care (TOC) is a crucial process for inpatient teams hoping to optimize patient experience and outcomes. Feedback from patients prior to leaving the hospital identifies several areas for improvement, as there are often misunderstandings about hospital courses and treatment plans. Such confusion leads to poor TOC. The Hospital Consumer Assessment of Healthcare Providers and Systems (HCAHPS) survey can be used as a marker of patient satisfaction and understanding of care.
Purpose: Increased satisfaction and adherence to treatment has been shown when patients are included in their disease management. Our teach-back process builds on this concept by providing an opportunity for patients to verbalize their plan of care. The crux of teach-back is to present small amounts of information and check for understanding daily (i.e. “chunk and check”). Beginning education from the day of admission improves physician and nursing communication with patients. The patient’s understanding of their diagnosis and follow-up plan can be assessed using an inpatient discharge survey. Adopting such a multifaceted approach contributes to enhanced patient health literacy and compliance; and has the potential to positively impact readmission rates as well as patient experience metrics.
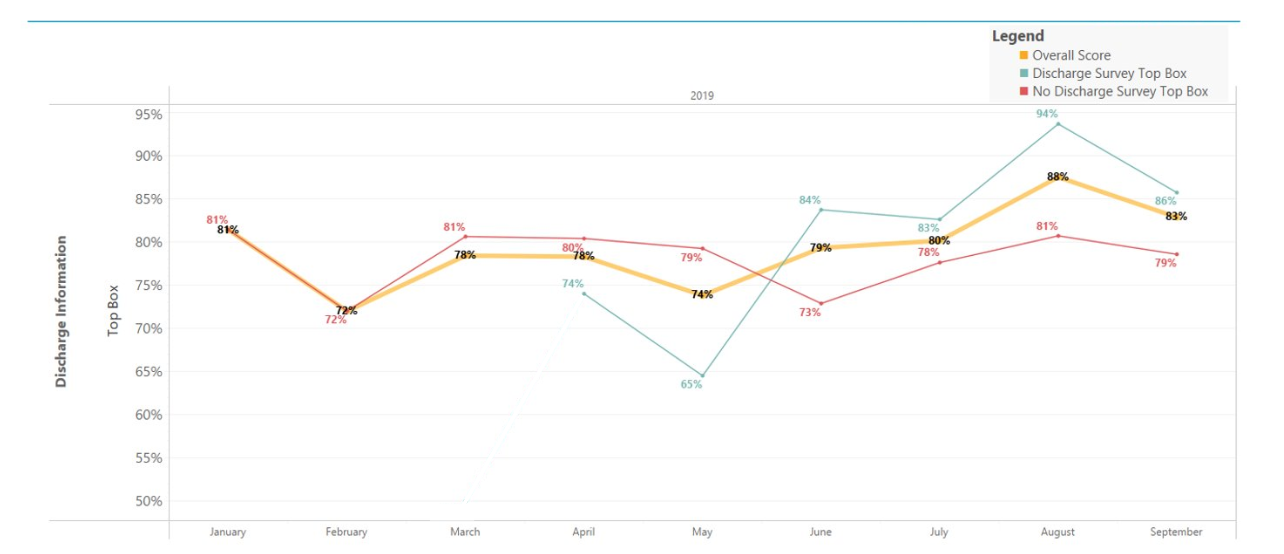
Description: Planning and communication are core to the teach-back and discharge survey process. The four points addressed during teach-back from admission to discharge are: (1) pertinent diagnoses, (2) medications, (3) symptoms that should prompt re-evaluation, (4) follow-up plan with outpatient providers. Teach-back requires the patient to summarize their diagnosis and hospital course in their own words. This is crucial in ensuring patients understand all aspects of their care and engages patients in their disease process.A team of physicians, nurses, and social workers responsible for monitoring the clinical progress of each patient identifies those ready for discharge. On the day of discharge, the physician meets with the patient to perform the final 4-point teach-back and answer questions. The nurse reviews discharge paperwork and administers a 4-question survey to the patient (through electronic tablets, Figure 1). Any knowledge gaps are addressed by the medical team and survey results are uploaded to Tableau (data visualization software). This teach-back and discharge survey process has currently been implemented on our regional medical/surgical floors. Our teach-back discharge initiative focuses on patient education through multidisciplinary conversations. The implementation of an electronic survey prior to discharge has helped maintain oversight of the process. Furthermore, we analyzed the efficacy of the teach-back discharge process by monitoring HCAHPS results. Data from April to September 2019 are shown in Figure 2. A maximum percentage increase of 22% in the discharge information of HCHAPS top box scores was noted amongst those who took the inpatient discharge survey.
Conclusions: The process of focused teach-back and inpatient discharge surveys are novel ways to approach provider to patient communication and TOC. Patients should be discharged with thorough knowledge of their disease process and follow-up plan. This process has already positively impacted patient understanding of discharge information. Ultimately, we hope that the continued practice of teach-back and inpatient assessment with electronic discharge surveys contributes to improved patient outcomes.