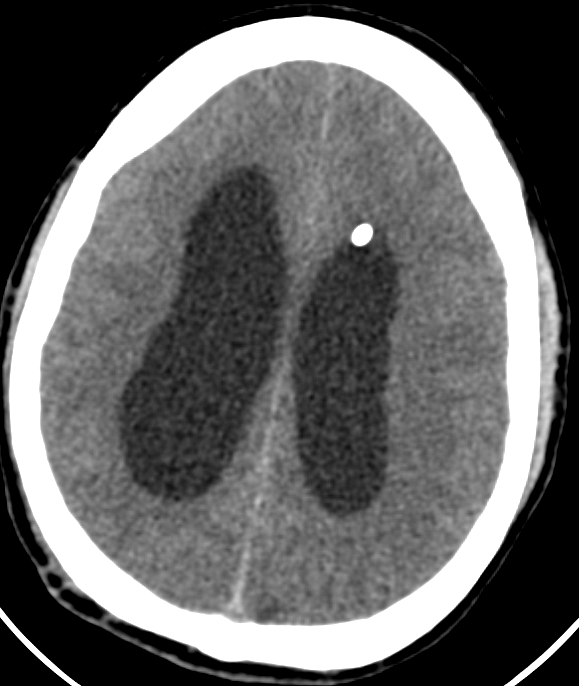
Case Presentation: 39-year-old male with history of previously treated TB meningitis 15 years ago, chronic hydrocephalus who received endoscopic third ventriculostomy few months ago, presented again with headaches and was found to have hydrocephalus. Patient received Ventriculoperitoneal shunt placement and CSF was obtained after the procedure. CSF studies showed (216-WBCs lymphocytic predominant fluid 81 %), elevated protein and low glucose but all the cultures were negative and meningitis/encephalitis panel was negative for HSV, CMV, cryptococcus, AFB. Patient evaluated by infectious disease and CSF abnormalities were attributed to post procedure sampling. A month later, patient presented again with abdominal pain and headaches. CT abdomen showed small collections in the abdomen not amenable to drainage. CSF sampling again showed lymphocytic predominant fluid with cultures consistent with mold which speciated as Histoplasma Capsulatum. HIV testing, serum and urine Histoplasma antigen testing was negative. On imaging there was no evidence of pulmonary involvement. VPS was removed; patient was treated with amphotericin B for six weeks and then was placed on fluconazole treatment. Multiple repeat CSF cultures remained negative. Repeat abdominal imaging showed resolution of intrabdominal collections. Of note this patient spent significant part of his life in Midwest United states and Mexico.
Discussion: CNS Histoplasmosis is an opportunistic infection in immunocompromised hosts affecting AIDS and transplant recipients. CSF involvement usually occurs in disseminated cases and encompasses subacute or chronic, meningitis, encephalitis, focal brain or spinal cord lesions (Histoplasmomas). Isolated CNS involvement in immunocompetent individuals is exceedingly rare. [1] Though cases have been reported secondary to VP shunt, this likely was not the case here because of preceding symptoms and suspicious CSF studies at the time of VPS placement. [2] Diagnosis can be challenging because culture data is usually negative and has limited sensitivity. Sensitivity can be increased by testing CSF histoplasma antigen and antibody in conjunction with CSF cultures. [4-6] Considering high relapse rates an aggressive and prolonged treatment approach is recommended with amphotericin for 6-12 weeks, followed by high dose fluconazole or Itraconazole for one year in immunocompromised hosts. [1]
Conclusions: This case illustrates the challenges in diagnosis of Histoplasma CNS infections because of a chronic course. Histoplasma CNS infection should be considered in presence of chronic symptoms suspicious of meningitis, equivocal CSF studies with negative culture data and patient origin from endemic areas.