Background: Electronic medical records have modernized healthcare by improving clinical efficiency, enhancing access to guidelines, and enabling decision-support tools. However, documentation features such as copy-forward and auto-population, while time-saving, can also perpetuate outdated or inaccurate information, contribute to “note bloat,” and obscure key clinical details (1). Prior studies demonstrate that standardized note templates and targeted educational interventions can improve documentation quality, reduce clutter, and enhance completeness (1–4). A QI project to enhance note quality and decrease note bloat was undertaken at our institution.
Methods: At our large urban, academic, quaternary care center, the internal medicine residents write progress notes (PNs) for patients on the Teaching Hospitalist service. A QI initiative to improve documentation included revising the existing PN template. To guide redesign, we surveyed key stakeholders, including residents and multidisciplinary team members (nurses, social workers, case managers, physical therapists, and nutritionists). Using this feedback, we created a new standardized PN template designed to reflect updated clinical information and reduce note bloat by removing imported, extraneous data available elsewhere in the chart. The new template was disseminated in 2025 and paired with a documentation didactic for incoming interns.Progress notes from the pre-intervention period (2024) were analyzed and compared with post-implementation notes. Process measures included the template uptake; outcome measures included the mean percentage of the note that was copied forward and the mean number of characters per note.
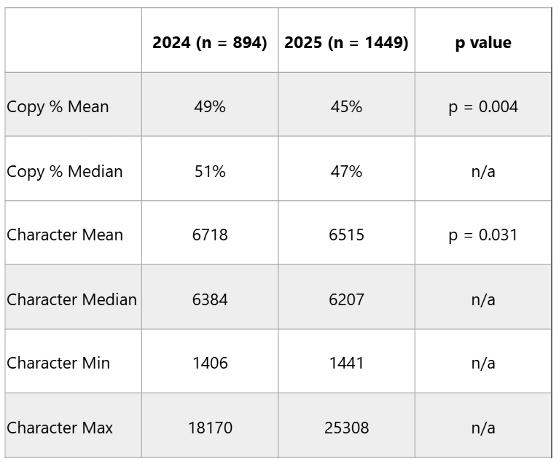
Results: Survey results showed that both residents and multidisciplinary staff felt notes were too long, prone to note bloat, and cluttered with extraneous information; only 62% of non-physician team members could clearly identify the active care plan. To address this, the revised progress note template included the top 3 priorities at the top of the note (fig. 1). To decrease note bloat, automated imports (e.g. labs, imaging, EKGs) were removed from the data section, instead prompting the writer to indicate what they actively reviewed. A total of 894 progress notes from July – September 2024 (pre-intervention) were compared with 1,449 notes from July – September 2025 (post-intervention). Following implementation, template uptake increased. The mean percentage of copied-forward content decreased from 49% in 2024 to 45% in 2025 (p = 0.004). Mean note length also significantly decreased from 6,718 characters pre-intervention to 6,515 characters post-intervention (p=0.031), indicating improved conciseness post-intervention (table 1).
Conclusions: Implementation of a redesigned progress note template paired with targeted education led to significant reductions in copied-forward content and overall note length. These findings suggest that standardized templates, when guided by stakeholder input and supported by education, can reduce note bloat and improve documentation quality. Notes still contained substantial copied material and remained lengthy, indicating that changing the template alone is insufficient to make notes lean. Additional provider education on lean documentation and creating a repository for outdated information are likely necessary to ensure notes are concise, current, and meaningful. These will be key focus areas for next steps in this QI initiative.