Background: Novel coronavirus (COVID-19) has resulted in over 1 million deaths globally(1). Prognostic tools to identify high risk patients are crucial to guide resource allocation efforts(2). We aimed at developing a risk assessment tool for patients with COVID-19 based on the risk factors with most significant effect on hospital admission and in-hospital mortality.
Methods: We performed a retrospective analysis of patients with positive COVID-19 that presented between 3/31/2020 – 5/15/2020 at Beaumont Health’s eight emergency departments (ED). The electronic health record (EHR) embedded risk score, previously externally validated, was modified based on risk factors with different points given to those that were statistically significant(2). Two outcome variables were measured, both using a yes/no binary scale: hospital admission and in-hospital mortality. Hospital admission, on the first encounter to the ED, was evaluated for the entire cohort, while mortality was evaluated only for inpatients that were discharged prior to 5/12/2020. Descriptive statistics, univariate/multivariate analyses by logistic regression were performed and presented as Adjusted Odds Ratios (AOR) with corresponding 95% confidence intervals and P-Values. P-Value < 0.05 was considered statistically significant. All analysis was done in SAS 9.4 (SAS Institute Inc., Cary, NC).
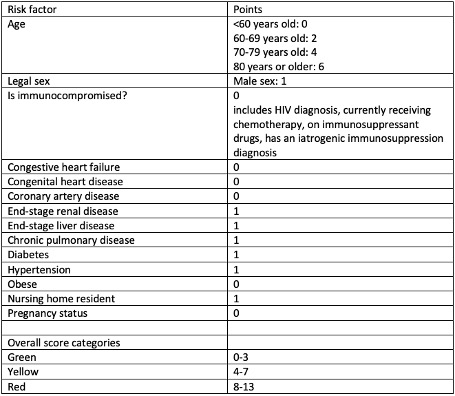
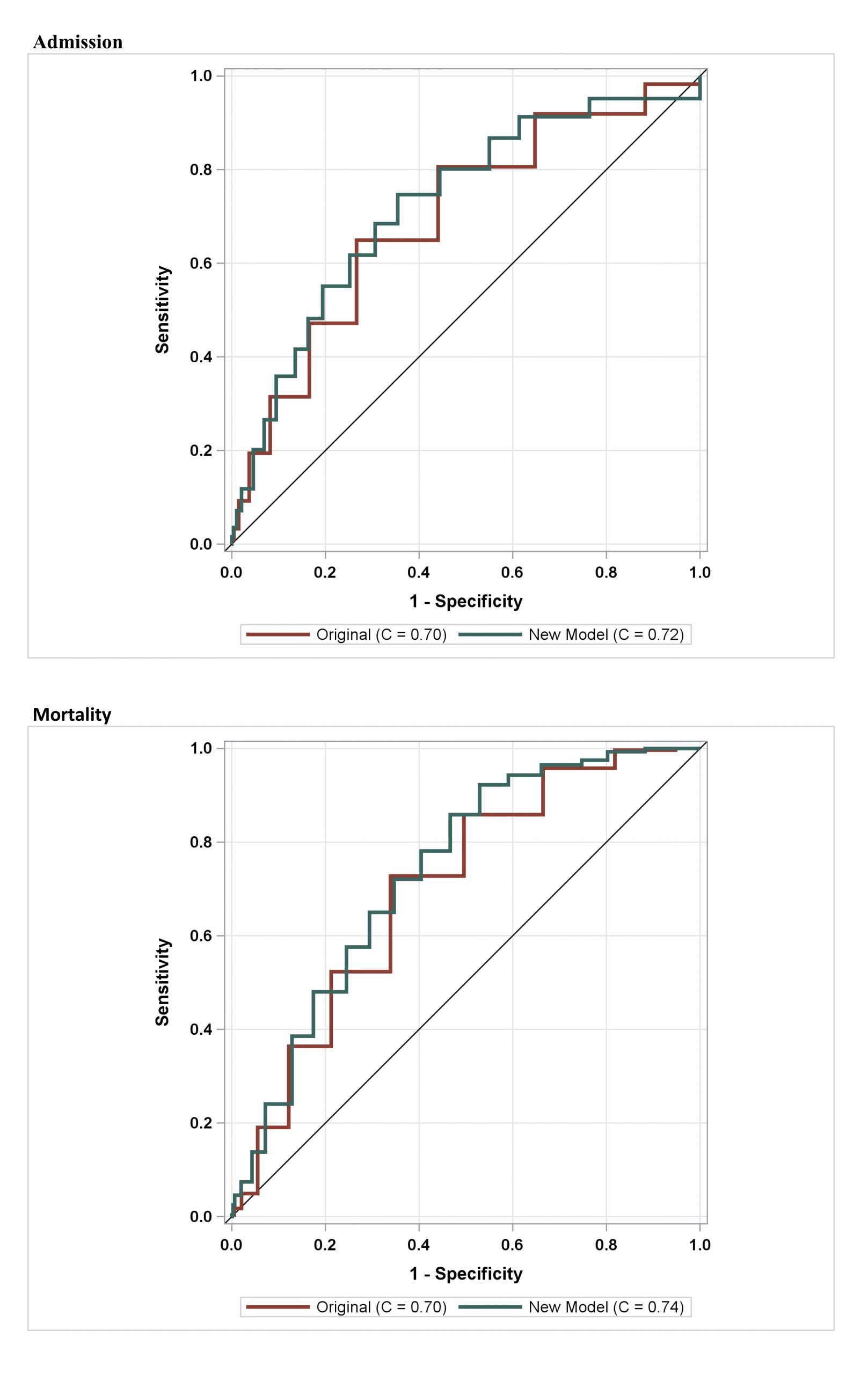
Results: 2,735 encounters with data extracted from EHR. 68.06% were hospital admissions, and 9.97% experienced in-hospital mortality. 61.23% were <69 years old. 58.07% had hypertension, 46.29% had chronic pulmonary disease, 37.81% had diabetes, and 6.71% had end-stage renal disease. Mean length of stay was 8.43 days. In the multivariate model to predict admission, end-stage renal disease (AOR 1.97), liver disease (AOR 7.77), chronic pulmonary disease (AOR 1.63), diabetes (AOR 1.70), hypertension (AOR 1.97), nursing home residence (AOR 1.90) were independently associated with admission. While immunocompromised, congestive heart disease, congenital heart disease, coronary artery disease, obesity had high odds of admission as well, there were no significant differences found. For prediction of in-hospital mortality in the multivariate model, chronic pulmonary disease (AOR 2.35), and nursing home residence (AOR 1.58) were significantly associated with in-hospital mortality. Other variables that had greater odds but were not significantly associated with in-hospital mortality included immunocompromised status, congestive heart failure, end-stage renal or liver disease, and obesity. Coronary artery disease, diabetes, and hypertension had lower odds of in-hospital mortality but did not meet statistical significance. The modified risk score recognized the statistically significant comorbid conditions and attributed no points to non-significant values. The cross-validated C-Statistics for the modified risk score model showed good discrimination for both admission (C=0.72) and in-hospital mortality (C=0.74) compared to the automatically generated risk tool for admission (C=0.70) and in-hospital mortality (C=0.70).
Conclusions: The modified risk score model created using statistically significant risk factors yielded a better scoring system than the scoring system automatically generated in Epic. This COVID-19 risk scoring model may help predict hospital admissions and in-hospital mortality for patients with COVID-19. Further external validation in a different cohort is recommended.