Background: Medical advances have improved survival for children with medical complexity (CMC), a growing population often dependent on medical devices and inpatient care provided by pediatric hospitalists. Existing literature has shown low resident confidence in caring for CMC, but no studies have examined pediatric hospitalists’ confidence, which may be a barrier to effective clinical teaching. This study aimed to assess pediatric hospitalists’ confidence in performing and teaching physical examination and device-related skills for CMC.
Methods: We administered a 25-question REDCap survey to a convenience sample of pediatric hospitalists responsible for resident supervision. This analysis reflects 9 questions (4 multiple-choice, 3 Likert-scale, 2 free-text) on demographics, self-confidence in performing and teaching complex care skills (physical examination maneuvers, identifying/describing, and troubleshooting devices), and barriers to teaching. Self-confidence was assessed using a 5-point modified Chen entrustment scale (scores 1-4 reflect increasing confidence performing a skill; 5 reflects confidence performing and teaching it). Descriptive statistics summarized quantitative data, and exploratory analyses examined associations between respondent characteristics and confidence. Free-text responses were grossly analyzed to determine predominant themes.
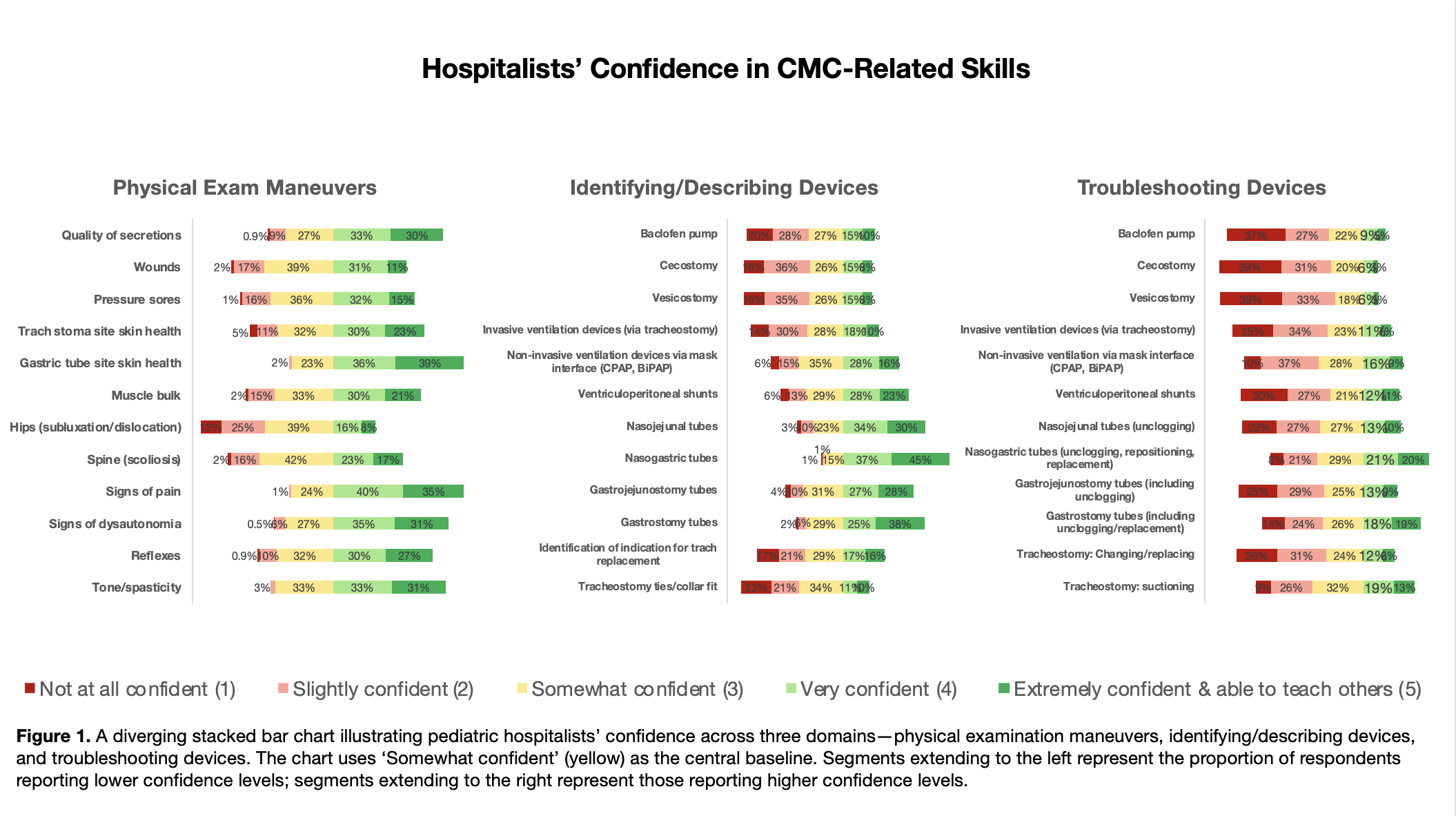
Results: Of 268 hospitalists surveyed, 221 (82.5%) responded, representing 53 institutions nationwide. Results are summarized in Figure 1. Mean overall self-confidence scores were 3.63 (SD 1.02) for physical examination skills, 3.22 (SD 1.26) for identifying/describing devices, and 2.56 (SD 1.25) for troubleshooting devices. Highest confidence was reported for assessing gastric tube site skin health (4.12, SD 0.83) and identifying/describing (4.24, SD 0.84) and troubleshooting (3.23, SD 1.23) nasogastric tubes. Lowest confidence was reported for hip examination (2.84, SD 1.09) and managing vesicostomies (2.02, SD 1.06) and cecostomies (2.03, SD 1.06). Fellowship training was significantly associated with greater confidence in identifying/describing (p=0.005) and troubleshooting devices (p=0.005). More years in practice correlated with higher confidence in neurologic and musculoskeletal examinations (p=0.041) but trended toward lower confidence in device management (p=0.077). Respondents with access to dedicated complex care providers reported lower confidence across all skills. Other than lack of self-confidence, respondents most frequently listed lack of time, resources, standardized curricula, and trainee interest as barriers to teaching CMC-related skills.
Conclusions: Pediatric hospitalists report variable confidence in physical examination and device management skills for CMC, with global difficulty teaching all measured skills. Fellowship training and years in practice appear to influence confidence positively in specific areas. These findings highlight a need for targeted faculty development initiatives to better equip hospitalists to prepare residents to provide high-quality care to CMC, particularly for experienced clinicians with limited device exposure during training.