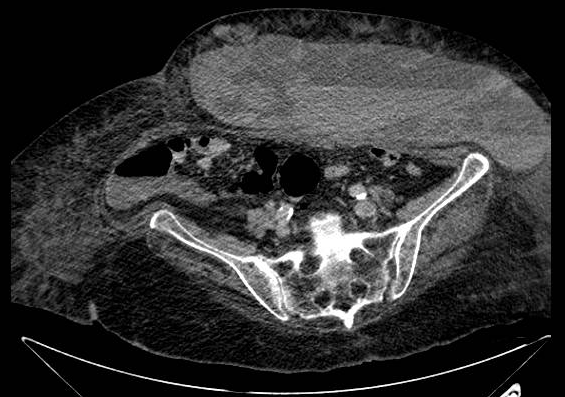
Case Presentation: An 88-year-old female with hypertension was admitted to the hospital due a to right tibiofibular fracture and underwent an open reduction internal fixation (ORIF). During admission, she was diagnosed with heart failure with preserved ejection fraction (>55%) and non-valvular atrial fibrillation with CHA2DS2-VASc score 5. She was started on therapeutic anticoagulation therapy for cardioembolic event prevention with enoxaparin 60 mg subcutaneously every 12 hours. One day during rounds, the patient began complaining of new, worsening left‐sided abdominal pain at the enoxaparin injection site associated with drowsiness, diaphoresis and fatigue. Physical examination and laboratories were remarkable for tachycardia, hypotension, a distended abdomen with generalized tenderness and a left upper quadrant area of induration and bruising associated with a hemoglobin drop from 9.3 g/dL to 5.4 g/dL. A diagnosis of hypovolemic shock was made and patient was resuscitated with intravenous fluids, packed red blood cells, and vasopressors. Abdominopelvic CT scan with contrast showed a large subcutaneous mixed density hematoma (2.9 cm x 7.6 cm x 10 cm) at the lower abdominopelvic wall with a hyperdense punctate focus within the hematoma suggestive of active bleeding. There was no identifiable source of bleeding and the left epigastric artery showed a normal course and caliber without evidence of extravasation of contrast to the hematoma. The patient was stabilized and transferred to intensive care unit for further hemodynamic support and close monitoring. Interventional Radiology and General Surgery services were consulted for acute management, but despite aggressive measures, the patient died of progressive bleeding during her ICU stay.
Discussion: Low-molecular-weight heparin (LMWH) is commonly used by physicians on a day-to-day basis as anticoagulation therapy for a multiple array of medical conditions (e.g. thromboembolism, atrial fibrillation, myocardial infarction) and deep vein thrombosis (DVT) prophylaxis. It is administered subcutaneously and often regarded as safe, but as any other pharmacological therapy, it is not exempt from serious and life threatening side effects that can have catastrophic consequences. Bleeding (13%) is the most common side effect, being intracranial hemorrhage the most likely site of lethal major hemorrhage. Abdominal wall or rectus sheath hematoma is an uncommon yet serious complication of anticoagulation therapies that can occur as a consequence of direct damage to the muscle or blood vessels. Nevertheless, this case proves that fatal major hemorrhage may occur in unexpected places and it is imperative for physicians to identify it early.
Conclusions: We describe a fatal subcutaneous hematoma in an elderly woman that occurred following abdominal injection of enoxaparin. We emphasize the importance of adequate training of the healthcare providers regarding subcutaneous enoxaparin administration as well as providing basic anatomical knowledge to avoid pitfalls leading to accidental arterial or muscular injury, and consequently, prevent dreadful life threatening abdominal wall hemorrhages.