Background: Physician Assistants (PAs) and Nurse Practitioners (NPs) play a growing role within hospital medicine groups. We studied physician perceptions of NPs and PAs in Hospital Medicine and identified factors that impact these perceptions.
Methods: Data was collected through a mixed methodology survey with both open and closed-ended questions on a 6 point Likert scale. An e-mail request to participate in the study, with personalized link to REDCap survey, was sent to physician hospitalists at 2 academic medical institutions in a large metropolitan area. Only providers who had direct experience working with NPs and PAs were encouraged to take the survey.
Results: The 25 respondents were physicians with an average of 6.2 years in practice. On average 40% of respondent clinical shifts were collaborative with NPs and PAs although 16% did not personally share patients with NPs and PAs. Survey response rate was 28.1%.
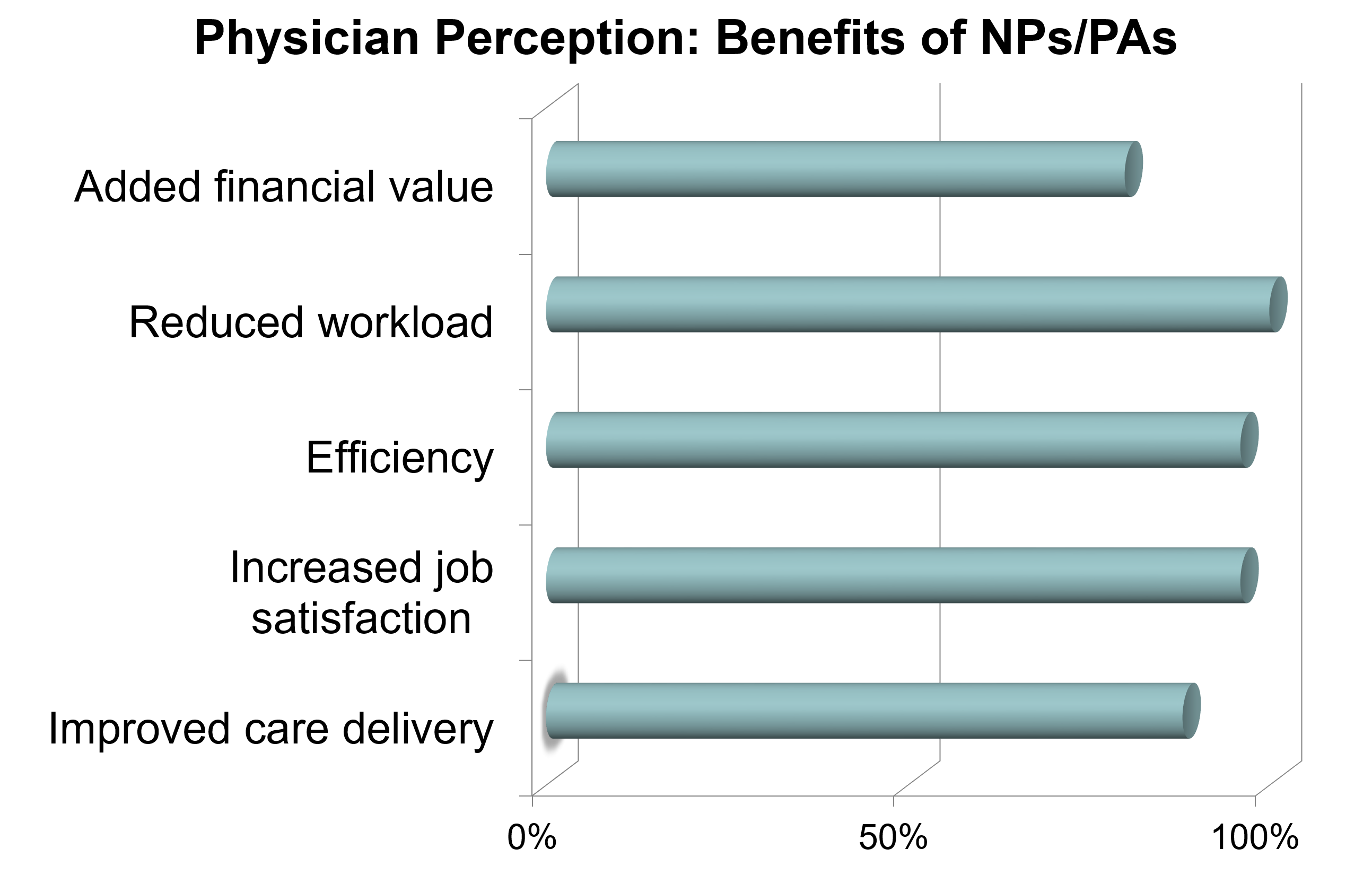
Ninety six percent (96%) agreed that inpatient teams benefit from having NPs and PAs (5.20, SD 1.19) and 88% felt that the patient care delivered by these teams was improved (5.16, SD 1.28). Ninety six percent (96%) reported working with NPs and PAs improved their own job satisfaction (5.16, SD 0.94). Ninety six percent (96%) agreed that this improves their own efficiency (5.36, SD 0.86) and 100% perceived it as reducing their workload (5.2, SD 0.76). Eighty percent (80%) reported NPs and PAs improve communication with patients (4.96, SD 1.14) versus 96% feeling they improve communication with other members of the healthcare team (5.2, SD 0.82). Eighty percent (80%) believed that NPs and PAs added financial value to the practice (4.48, SD 1.33). The median respondent believed NPs and PAs function most similar to 3rd year residents and care for a census approximately 75% of a physician in their group. Ninety two percent (92%) prefer working with NPs and PAs with multiple years of clinical experience (5.2, SD 1.03) but 96% would prefer to work with NPs and PAs who have participated in additional training beyond PA/NP school (5.4, SD 0.91).
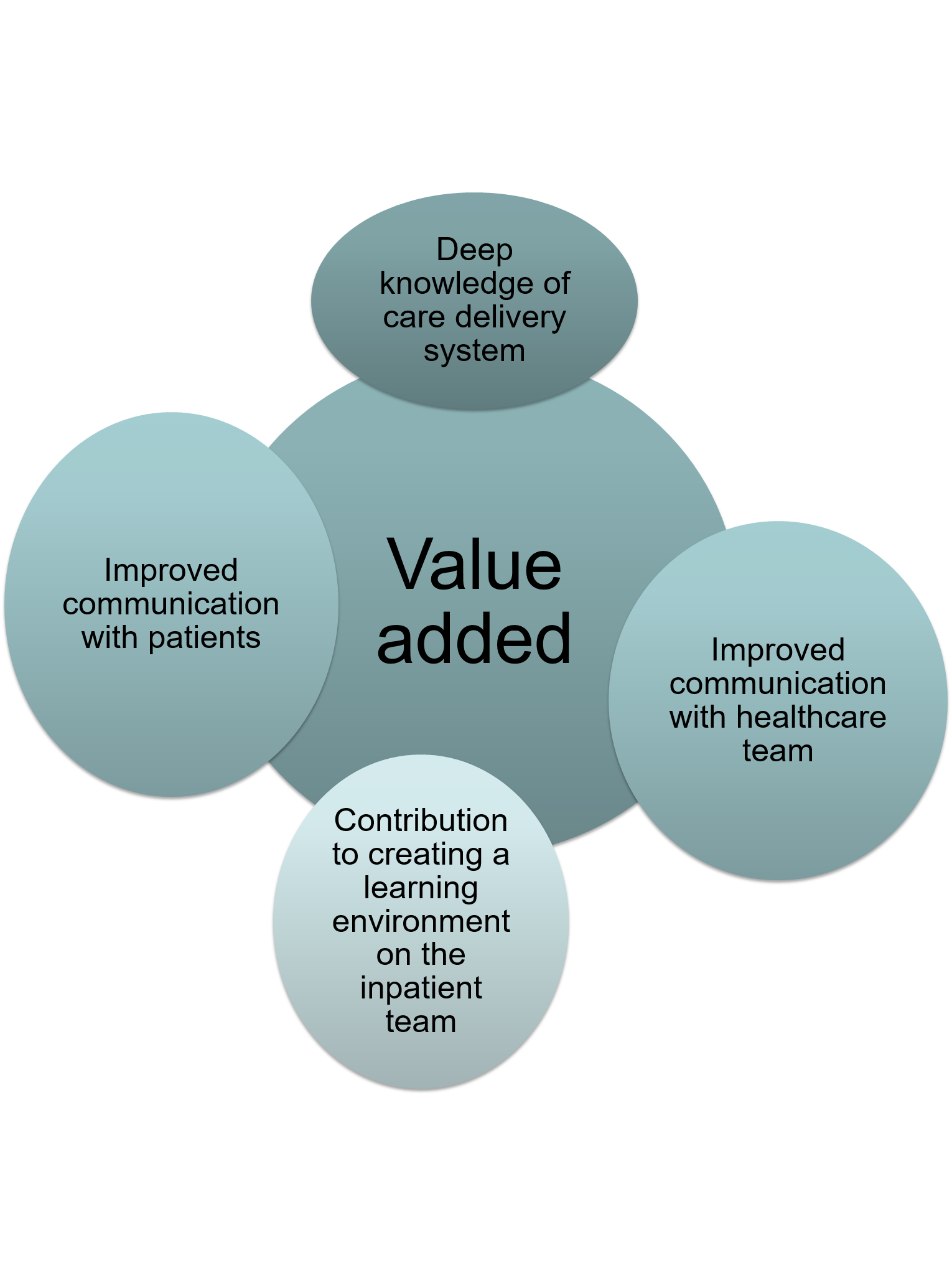
Free text responses to questions about the value provided by NPs and PAs revealed many of the anticipated domains of value including being efficient clinicians, functioning well on teams, and communication skills. The comments also revealed aspects of value not anticipated including personal characteristics, positive interpersonal interactions, and deep knowledge of the care delivery system. One recurring theme was how the presence of NPs and PAs contributes to creating a positive learning environment on the inpatient team and the value created by having multiple clinicians having input into a complex patient’s care. By sharing workload the perception was that patients receive more time from clinicians at their bedside.
Conclusions: The perceptions by hospital medicine physicians of NPs and PAs were nearly universally positive. Notable were the positive impacts PAs and NPs had on physician perceptions of the clinical care provided, practice efficiency and provider satisfaction.