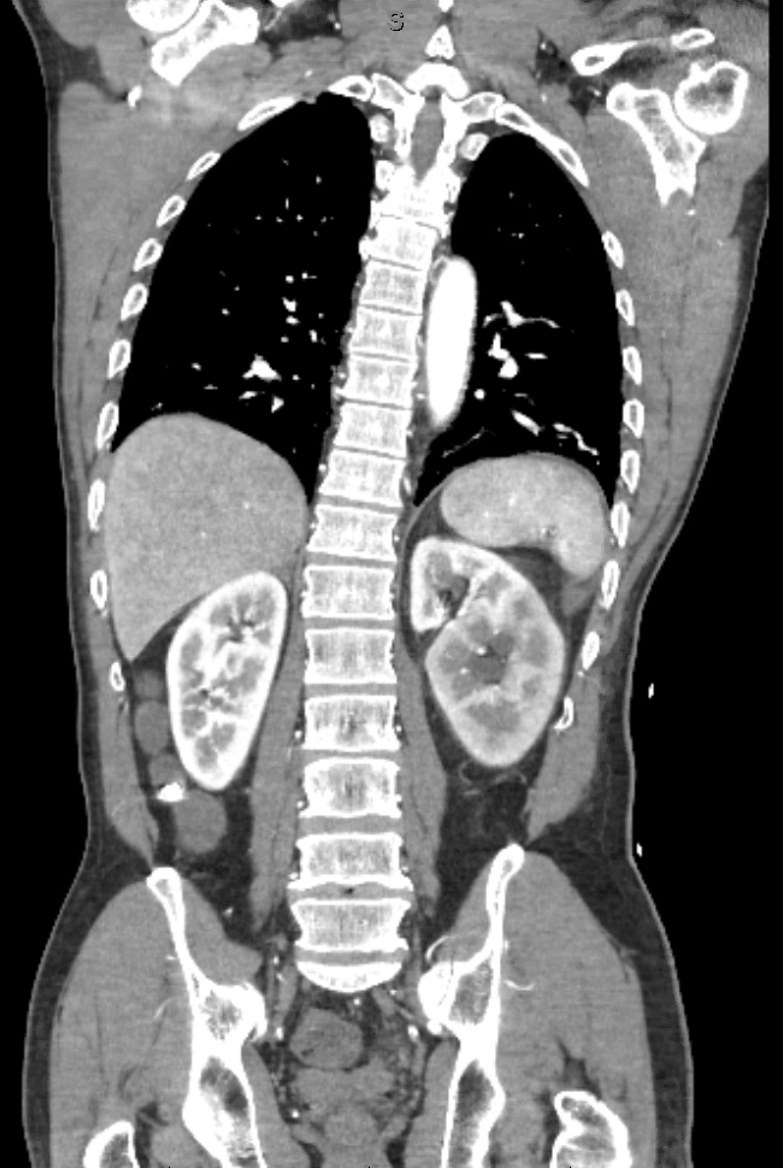
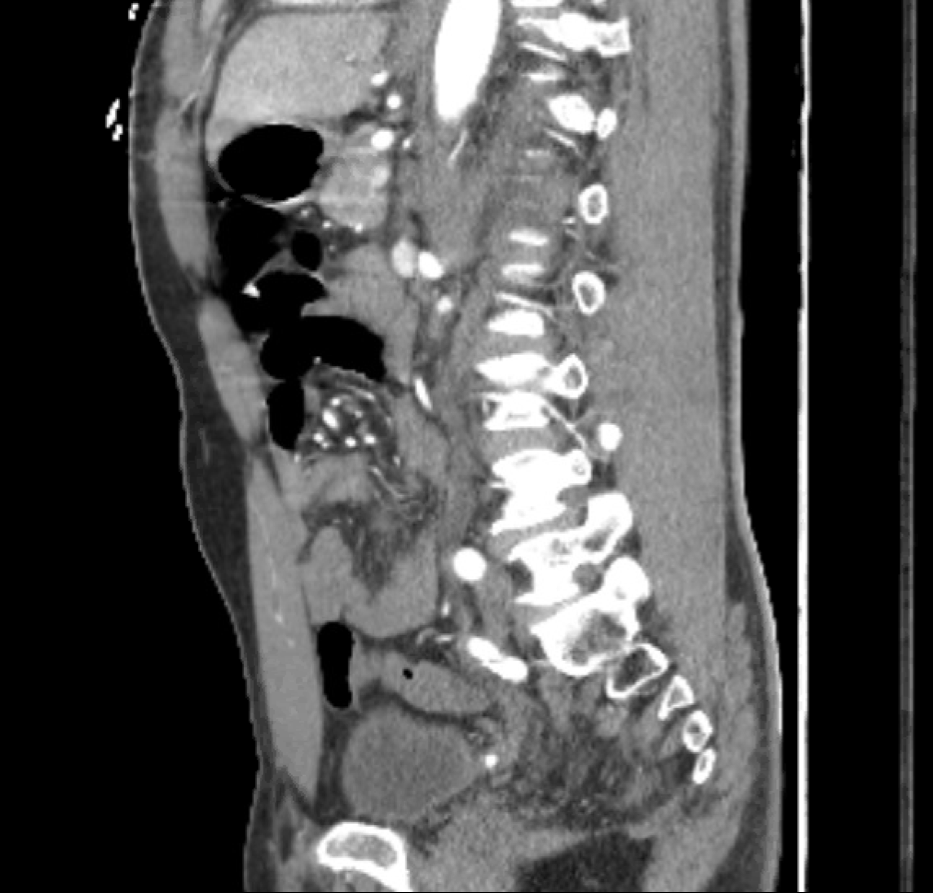
Case Presentation: A 67-year-old male with a past medical history significant for hypertension and a prior cerebrovascular accident presented with subjective 9/10 left-sided abdominal pain, systolic blood pressure >200, and tachycardia. Upon presentation, the patient experienced several episodes of asymptomatic supraventricular tachycardia. Blood work subsequently drawn showed no elevated troponins. After the second episode of supraventricular tarchycardia, a CT dissection protocol was initiated that showed no dissection. However, it uncovered a hyperechoic region of the left kidney, suggesting a renal infarct versus renal congestion. It also demonstrated a retroaortic left accessory renal vein that was potentially compressed between the aorta and the vertebral column. Additionally, the patient’s creatinine was 1.6, increased from his baseline of 1-1.2, and a urinalysis was notable for hematuria and proteinuria. The patient was admitted to medicine for further work up of his acute kidney injury and possible renal infarct.A subsequent doppler ultrasound showed patent venous flow through the left main renal vein despite suspected compression of the accessory vein. Imaging was reviewed by vascular surgery who recommended no emergent surgical intervention. The patient was stabilized, with his blood pressure controlled, pain managed, and creatinine normalized with IV fluids. The CT dissection imaging was reviewed in greater scrutiny with both medical and radiology staff, and it was recognized that the patient had two left-sided ureters and a 4x4mm nonobstructing urolith near the uretovesicular junction. His management was adjusted, and he was discharged on tramadol for pain management and instructions to hydrate well.
Discussion: This patient’s presentation of left flank pain, hematuria and proteinuria, and severe hypertension, with a CT read suggesting renal infarct and a compressed retroaortic renal vein, was consistent with renal infarct secondary to posterior nutcracker syndrome. However, posterior nutcracker syndrome is exceedingly rare and a diagnosis of exclusion. Our patient’s CT illustrated a likely compressed accessory renal vein, but it also showed a hyperechoic region of the left kidney that did not correspond to the area that was associated with the renal vein in question, according to one of the reads. Due to this discrepancy and the unusual presentation of our patient, we sought diagnostic clarity in the form of an integrative team and were eventually able to visualize the urolith.
Conclusions: We have demonstrated a case of a patient with a retroaortic accessory renal vein and a clinical picture consistent with posterior nutcracker syndrome who was ultimately found to have a kidney stone. This emphasizes the need to incorporate a broad differential to avoid anchoring bias when presented with a possible rare diagnosis, as well as the utility of interdisciplinary review of potentially rare radiological findings.