Background: Kidney Dialysis is a vital treatment for patients with end-stage renal disease. But lately, there has been an alarming increase in deaths related to this procedure. This study analyzed mortality trends and disparities among adults aged 15 and older from 1999 to 2020.
Methods: The study examined post- kidney dialysis complications-related mortality in the United States from 1999 to 2020 using death certificate data from the CDC WONDER database, focusing on cases classified under ICD-10 code Y84.1. Age-adjusted mortality rates (AAMRs) per 100,000 individuals were analyzed to identify trends over time. Joinpoint regression was employed to estimate the Average Annual Percent Change (AAPC) and assess statistical significance through p-values. Mortality patterns were further explored by stratifying the data across variables such as year, sex, race/ethnicity, and geographic regions.
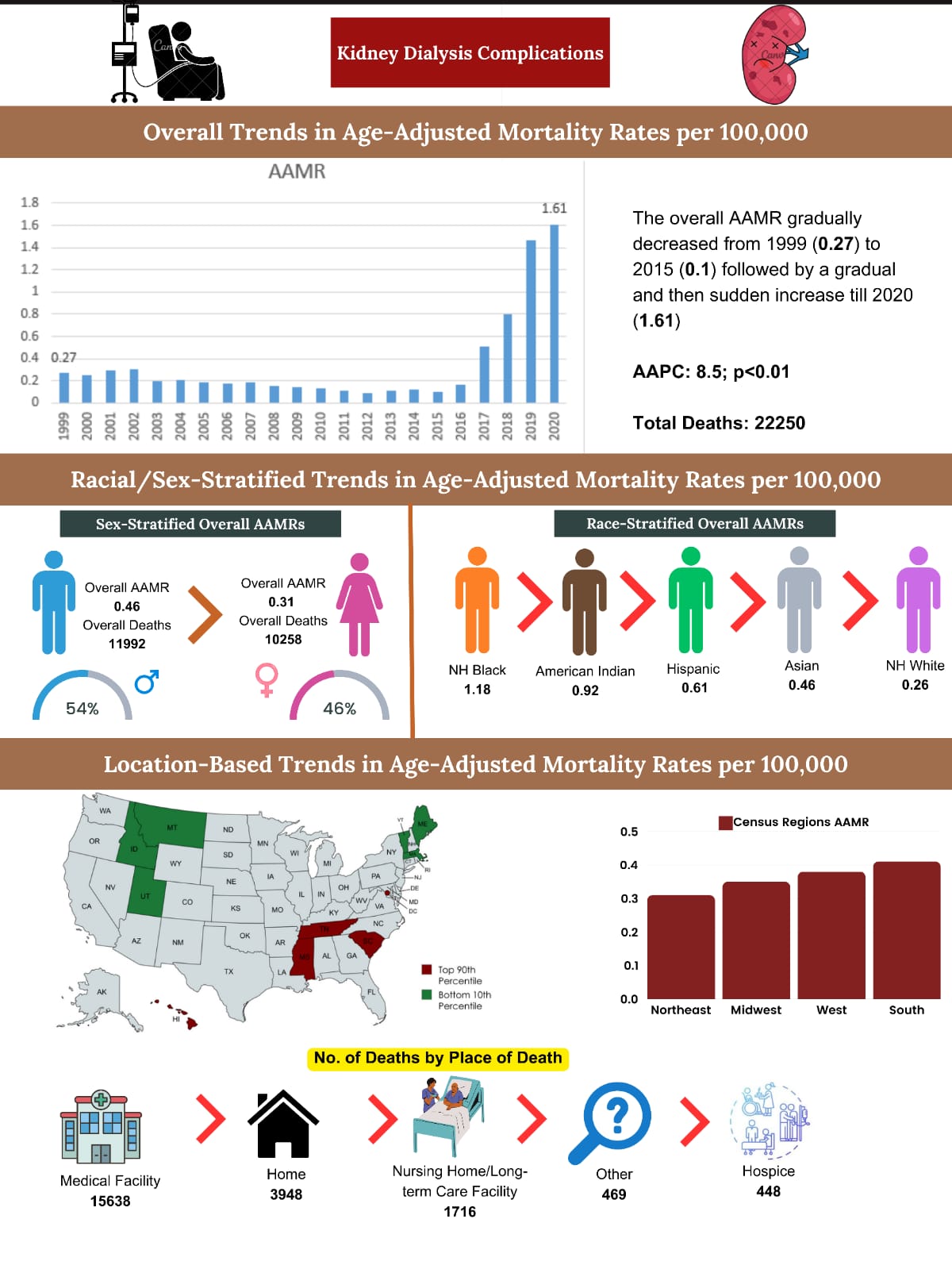
Results: From 1999 to 2020, kidney dialysis complications were responsible for 22,250 deaths among U.S. adults aged 15 and older. The majority of these fatalities occurred in medical facilities (70.0%), with descendent’s homes accounting for 17.7%. The age-adjusted mortality rate (AAMR) increased nearly sixfold, rising from 0.27 in 1999 to 1.61 in 2020, with an average annual percent increase (AAPC) of 8.5 (p< 0.01). Men had higher AAMRs than women (0.46 vs. 0.31) plus the rate of increase was also slightly higher for men (AAPC: 9.2, p< 0.01) compared to women (AAPC: 8.1, p< 0.01). Significant racial disparities were noted: non-Hispanic (NH) Blacks had the highest AAMR (1.18), followed by NH American Indians (0.92), Hispanics (0.61), NH Asians or Pacific Islanders (0.46), and NH Whites (0.26). Hispanics experienced the steepest increase over time (AAPC: 9.9, p< 0.01). Geographically, District of Columbia recorded the highest state-level AAMR (0.94), while Montana had the lowest (0.15). Among U.S. regions, the South led with the highest AAMR (0.41), followed by the West (0.38), Midwest (0.35), and Northeast (0.31). Rural areas had slightly higher AAMRs than urban ones (0.38 vs. 0.37), with both rural and urban areas having similar rates of increase over time (AAPC: 8.6, p< 0.01).
Conclusions: This study uncovers substantial disparities in kidney dialysis related mortalities among US adults. The shocking sixfold increase in mortality rates requires immediate attention for targeted interventions and changes in policies. These discoveries highlight the need for a drastic change in kidney dialysis procedure guidelines and enhanced education of healthcare professionals to decrease mortality trends in the future.