Background: The transition from adolescent to adult care has been associated with worse outcomes including increased mortality (1). Improved patient experience (PEX) correlates with decreased inpatient mortality rates and better adherence to quality guidelines (2) as well as lower 30- day readmission rates for patients with heart failure, acute MI and pneumonia (3). Hospitalized adolescents have unique psychosocial needs that impact their inpatient experience and challenge the patient-provider relationship (4-6). Young adults transitioning from pediatric units to adult units in hospitals encounter different environments, cultures and processes of care. Accordingly, young adults may experience care differently than other hospitalized adults.
Methods: We performed a retrospective cohort study using a national, de-identified patient experience dataset collected via Press Ganey (PG) surveys between January 1, 2017 and December 31, 2019. We described and compared survey responses across all aspects of the hospital stay for inpatients aged 14-29. Composite scores for the 10 domains, or facets, of the hospital stay, were obtained by calculating the mean score from each domains’ questions. Composite scores for each health facility were converted to percentile rankings, which were then used to compare percentile rankings of the domains by age group. Hospitals that contributed less than 30 surveys were excluded from percentile rankings. All analyses were performed using SAS version 9.4. P-values <0.05 were considered statistically significant.
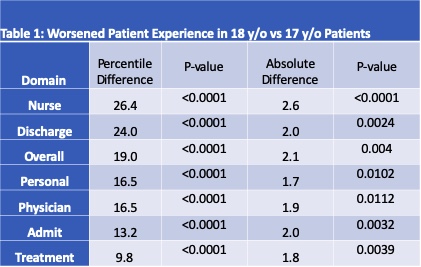
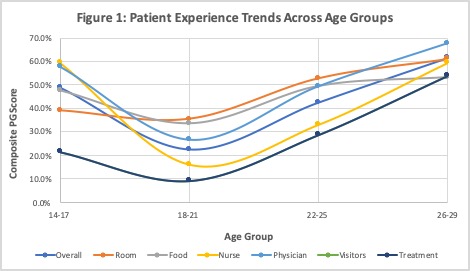
Results: We evaluated the results of 174,174 PG patient experience surveys across a national sample of US hospitals. The surveys include 25,354 from teaching, 127,969 from non-teaching and 20,851 from academic hospitals. When comparing the patient experiences between 17-year-olds (y/o) (n=1022) and 18 y/o (n=4054) patients, 18 y/o rated experience with physicians (16.5 difference, p<0.0001) and nurses (26.4 difference, p <0.0001) worse than 17 y/o. In addition, 18 y/o rated hospitals lower for admission and discharge processes, with percentile differences of 13.2 (p <0.0001) and 24 (p<0.0001) respectively. Overall, 18 y/o hospital percentile ratings were 19 percentiles worse than 17 y/o (p <0.0001) Table 1.When comparing factors that led to a higher PG score category for 14-17 y/o, non-teaching hospitals demonstrated lower odds of higher PG scores (OR 0.71, p= 0.01) compared to academic hospitals. For 18-21 y/o, there was also a significantly lower odds of a better PG scores for non-academic hospitals (teaching OR 0.87 p=0.01; non-teaching OR 0.85 p=0.002). Moderately sized hospitals (250-499 beds) also demonstrated a decreased odds of a higher PG scores when compared to small (<100 bed) hospitals (OR 0.66, p= 0.02). Nearly every facet of patient experience saw a significant decline between ages 14-17 and 18-21. (Figure 1).
Conclusions: In a national sample of PG PEX surveys, hospitalized adolescents and young adults experienced worse patient care regardless of hospital type. In particular, our results demonstrate that 18 y/o report dramatically worse PEX percentile rankings compared to 17 y/o in nearly every domain. By ages 26-29, PEX appears to have rebounded to pre-18y/o levels. These results call for further investigation to elucidate the unique needs of hospitalized adolescents and young adults and to develop strategies to improve their inpatient experiences.