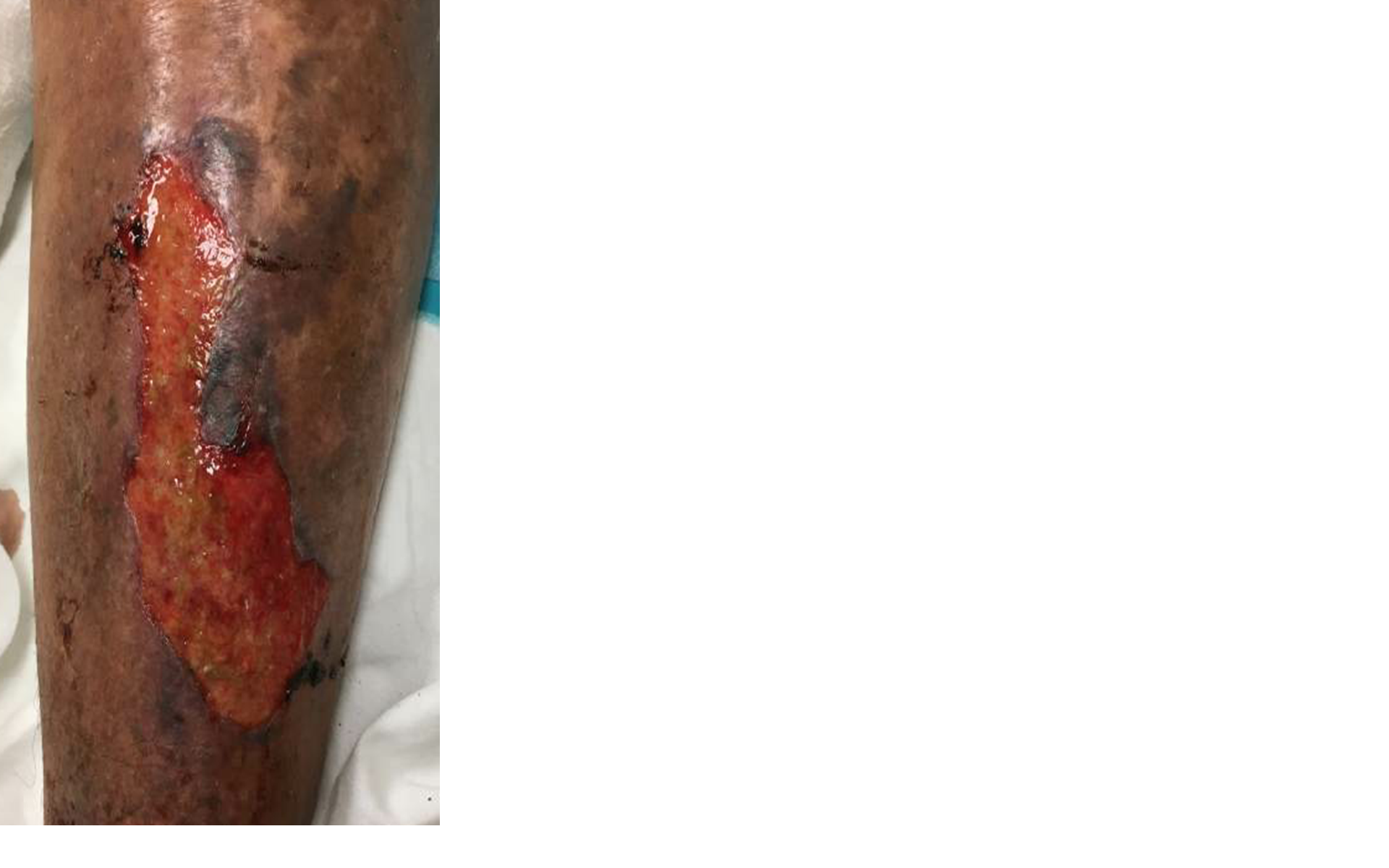
Case Presentation: The patient is a 67 years old female with Hepatitis C and alcoholic liver cirrhosis, HCC, atrial fibrillation who presented to the ED with fever, chills and altered mental status. Per husband, the patient did not have any focal symptoms including cough, abdominal pain, burning urination, headache or photophobia. On initial evaluation patient’s T 39.7 °C, BP 76/62 mmHg, HR 144, SpO2 98% in ambient air. Her cardiac examination revealed S1, S2 with no murmurs, lung examination revealed bilateral air entry with no added sounds, the abdomen was soft with no rebound or rigidity. Examination of the skin revealed extensive abrasion in the left lower extremity, the cause of which was not known at the time of admission. However, there were no signs of cellulitis at the site of abrasion. Initial laboratory investigations revealed leucocytosis, lactic acidosis, elevated liver enzymes. Imaging of the chest and abdomen did not reveal any focus of infection. The patient was volume resuscitate d and started on broad spectrum antibiotics. Blood culture eventually grew Pasteurella multocida. Antibiotics were de-escalated to ampicillin-sulbactam, repeat cultures were negative. The patient had improved clinically, antibiotics were switched to amoxicillin-clavulanate and recommended to complete 14 days of antibiotic therapy. The patient later admitted to having more than twenty cats in her house and two aggressive cats had scratched her legs a few days prior to the presentation.
Discussion: Pasteurella multocida is a commensal bacteria in the respiratory and gastrointestinal tracts of cats and dogs. Human transmission from the pets occurs mainly due to animal bites and typically leads to cellulitis, rarely it can lead to bacteremia especially in immunocompromized hosts. The number of households in urban United States with pets has been on the rise. Here, we report a case of Pasteurella multocida in a patient with cirrhosis and hepatocellular carcinoma (HCC).
Although Pasteurella multocida bacteremia has been reported in immunocompetent hosts, it is more common in immunocompromized hosts, especially in patients with cirrhosis, hematological malignancies, and organ transplant. It is important to be aware of this disease in patients presenting with unexplained sepsis and have animal exposure, especially in immunocompromized hosts. In a case series of patients with Pasteurella multocida bacteremia, 77% of patients were found to have underlying cirrhosis. Our patient had cirrhosis and hepatocellular carcinoma as the underlying predisposing factor.
Conclusions: 1. It is important to be aware of this disease in patients presenting with unexplained sepsis and have animal exposure, especially in immunocompromized hosts.
2. Immunocompromized patients should be educated on the risk of Pasteurella multocido sepsis with animal bite.
3. Like Vibrio vulnificus, there might be a mechanistic association between Pasteurella multocida and cirrhosis. It is worth exploring the association between cirrhosis and Pasteurella multocida bacteremia.