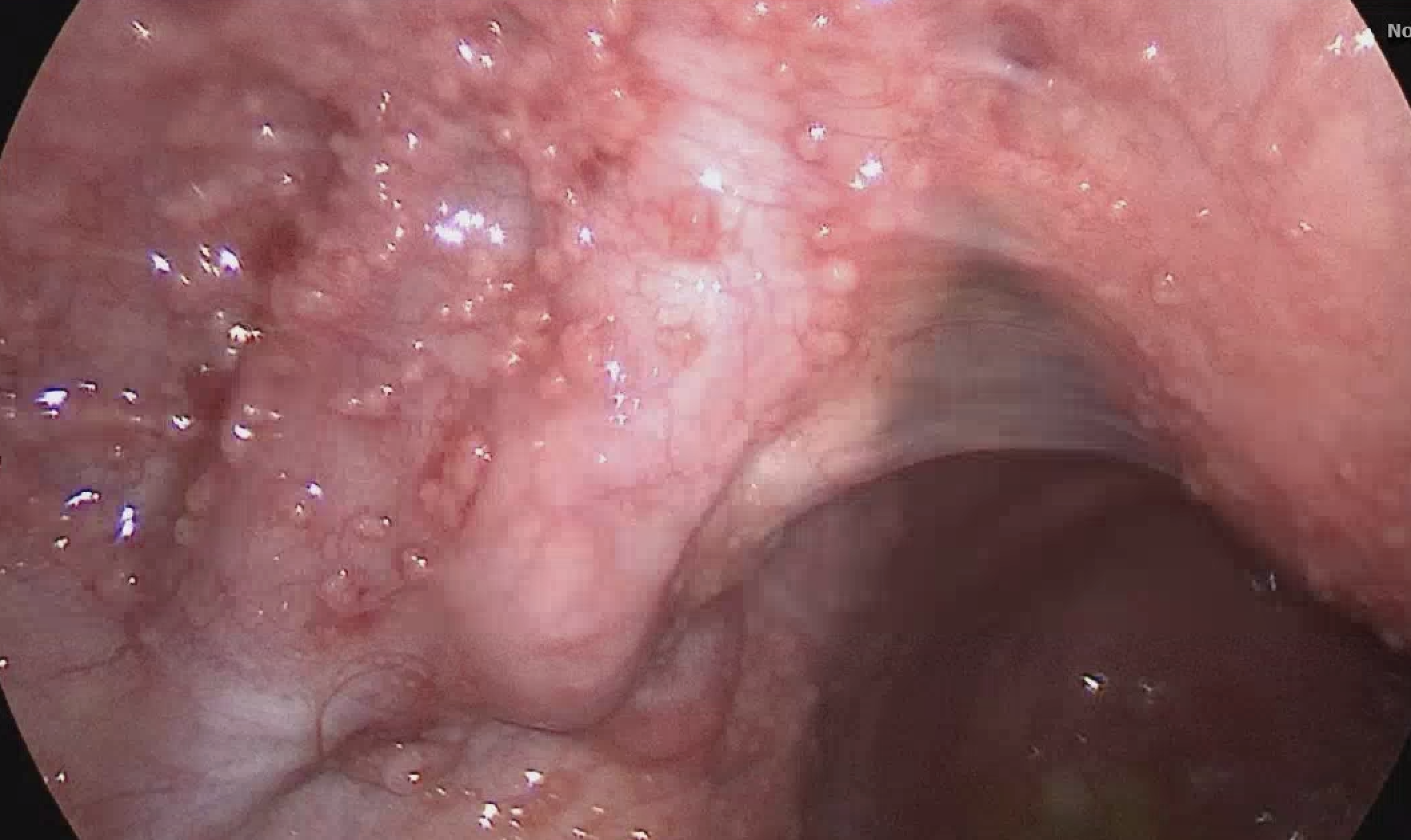
Case Presentation: A 36-year-old woman, a missionary from Papua New Guinea with a history of nonalcoholic hepatic steatosis, presented with new-onset abdominal pain, early satiety, and progressive abdominal distension. She denied alcohol, tobacco, or drug use and had no prior malignancy screening. Physical examination revealed a protuberant abdomen with a fluid wave but no lymphadenopathy. Computed tomography (CT) showed hepatosplenomegaly, large volume ascites, omental thickening, small bowel edema, and a left pleural effusion. Tumor markers revealed an elevated CA-125 of 701 U/mL (reference 0-35 U/ml), with normal CEA, AFP, and CA 19-9, raising suspicion for ovarian malignancy or Meigs syndrome. Cytologic analysis from paracentesis and thoracentesis was negative for malignant cells. Diagnostic laparoscopy revealed greenish ascitic fluid and diffuse peritoneal nodularity resembling carcinomatosis. Biopsies showed necrotizing granulomatous inflammation with multinucleated giant cells. Special stains for fungi, bacteria, and spirochetes were negative. Acid-fast bacilli (AFB) staining was positive for a single organism, and PCR confirmed Mycobacterium tuberculosis complex.Initial QuantiFERON TB was negative, with positive repeat testing; HIV testing was negative, as well as three sputum AFB cultures. The patient was diagnosed with peritoneal tuberculosis and treated with rifampin, isoniazid, pyrazinamide, and ethambutol for two months, followed by isoniazid, rifampin, and pyrazinamide for four months, per the Infectious Disease specialist. The county health department supervised therapy and follow-up.
Discussion: Peritoneal tuberculosis occurs through hematogenous spread, ingestion of infected material, or extension from adjacent foci. Although rare in developed nations, it remains prevalent in endemic regions such as Papua New Guinea, where TB notification rates exceed 700 per 100,000 population, with a high proportion of extrapulmonary disease. [1] Clinical presentation is nonspecific—ascites, abdominal pain, weight loss, and elevated CA-125 often mimic ovarian malignancy.Diagnosis is challenging due to the low sensitivity of AFB smear and culture from ascitic fluid (21–69%). Laparoscopy with targeted biopsy remains the diagnostic gold standard, revealing caseating granulomas and AFB positivity. [2,3,4,5] Elevated CA-125 reflects peritoneal irritation rather than malignancy. Early recognition is essential to avoid unnecessary oncologic surgery and to initiate curative anti-TB therapy promptly.
Conclusions: This case underscores the diagnostic complexity of peritoneal tuberculosis presenting as pseudo–ovarian carcinoma. In patients from TB-endemic regions with ascites, pleural effusion, and elevated CA-125, clinicians must maintain a high index of suspicion for TB. Definitive diagnosis relies on histopathology and microbiologic confirmation via peritoneal biopsy.For hospitalists, often the first providers to evaluate patients with unexplained ascites or systemic symptoms, recognizing peritoneal tuberculosis as a malignancy mimic is vital. Early inclusion of TB in the differential diagnosis can prevent invasive procedures, expedite targeted testing, and ensure timely initiation of anti-tubercular therapy. Awareness of this presentation allows hospitalists to coordinate multidisciplinary care efficiently and improve outcomes.
.png)