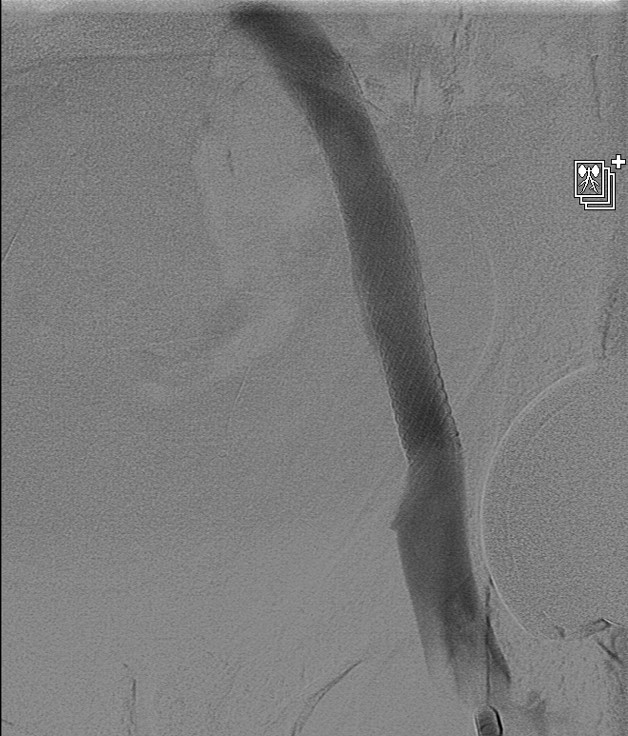
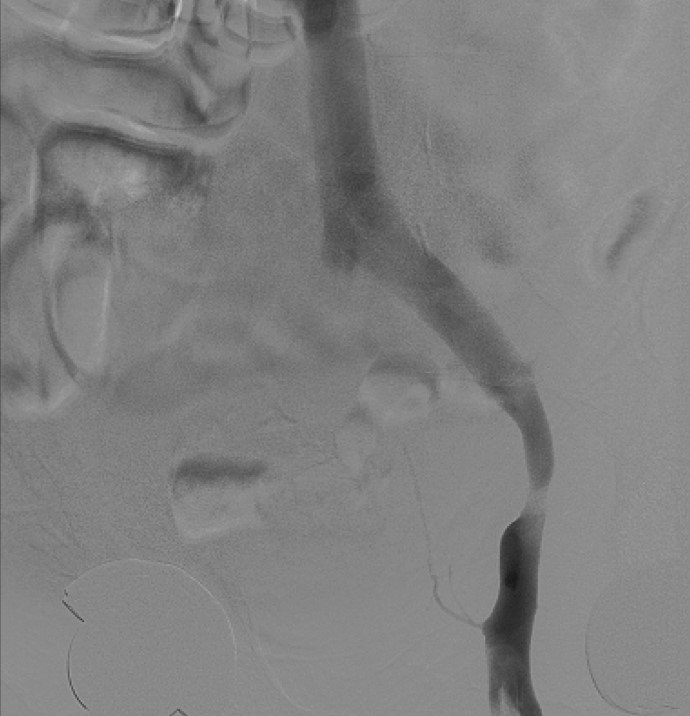
Case Presentation: A 59-year-old male patient with no significant past medical history presented to our hospital with left foot swelling that started almost four weeks prior to presentation. The swelling was progressive, ascending, and associated with erythema. The patient was initially evaluated by his primary care physician who requested a venous Doppler of his lower extremity. This was negative for deep venous thrombosis (DVT), and he was subsequently started on a course of antibiotics due to concern for cellulitis. Despite antibiotic therapy, the patient’s swelling progressed to involve the entire left lower extremity. The patient was started then on conservative venous insufficiency treatment including compression stockings, leg elevation, and later Lasix. Given the patient’s persistent symptoms and lack of improvement despite those measure, he was referred for a venogram which showed patent venous system in the right side but revealed a narrowing in his left external iliac vein, the area of stenosis occurred at the crossing of what looked like a pulsatile artery, at the level of the crossing of the hypogastric artery into the pelvis. The patient underwent angioplasty and stenting of the narrowed vein which he tolerated well. He was later discharged on aspirin, clopidogrel, and a short course of antibiotics, and his swelling resolved completely three weeks later.
Discussion: We present a case of a middle age male who was evaluated for progressive unilateral lower extremity edema. After ruling out DVT, he was managed conservatively but his symptoms failed to improve which led to further diagnostic testing which revealed a diagnosis of a rare variant of May-Thurner syndrome (MTS). MTS is an anatomically and pathologically variable condition leading to venous outflow obstruction as a result of extrinsic venous compression in the iliocaval venous territory. With partial venous obstruction, the condition can be asymptomatic, but progression with symptoms related to chronic venous hypertension or venous occlusion can occur, with or without venous thrombosis. It is important to keep this condition in mind whenever a patient presents acutely with lower extremity swelling or (DVT), particularly young women.
Conclusions: This case has two educational objectives, the first of which is the presentation of a rare variant of May-Thurner syndrome which caused unilateral lower extremity swelling in an otherwise healthy middle-age man. This syndrome is usually caused by compression of the left common iliac vein by the overlying right common iliac artery, but in this case, it was caused by the hypogastric artery which is extremly rare. Second, this case demonstrates the importance of keeping a wide differential diagnosis, and to look for the underlying etiology especially in cases of a unilateral lower extremity swelling. The discovery of his anatomical pathology led to the appropriate management of his symptoms, which would have otherwise persisted in the setting of conservative management.