Case Presentation: A 75-year-old woman with hypertension, hypothyroidism, and rheumatoid arthritis on Methotrexate (MTX) and prednisone, recently hospitalized for right foot cellulitis treated with Bactrim, presented after her neighbor found her confused and unable to move. On arrival, she was somnolent, tachycardic to 130, hypotensive to 98/50, and reported several weeks of diarrhea and painful oral intake due to worsening mouth soreness. She endorsed routine MTX use but was unsure of the dose or schedule. Exam showed cachexia, oral mucositis of the hard palate, a systolic murmur, and a non-infected right foot wound. Labs revealed Na 162 mEq/L, Cr 1.6 mg/dL (baseline 0.6 mg/dL), BUN 87 mg/dL, WBC 0.9 x 10^6/L, Hgb 13.0 g/dL, MCV 118 fL, Plt 76 x 10^6/L, AST 47 U/L, and ALT 39 U/L. Routine labs three weeks earlier were normal. HIV, HCV, and B12 were normal. Folate was low (3.7 ng/mL). MTX level (Ark Diagnostics) on hospital day two was undetectable. Further history revealed inadvertent MTX ingestion three times daily instead of weekly. Despite a normal MTX level, her presentation was consistent with MTX toxicity. MTX was held and oral folic acid started. Her WBC improved, platelets stabilized, and mentation normalized by hospital day four.
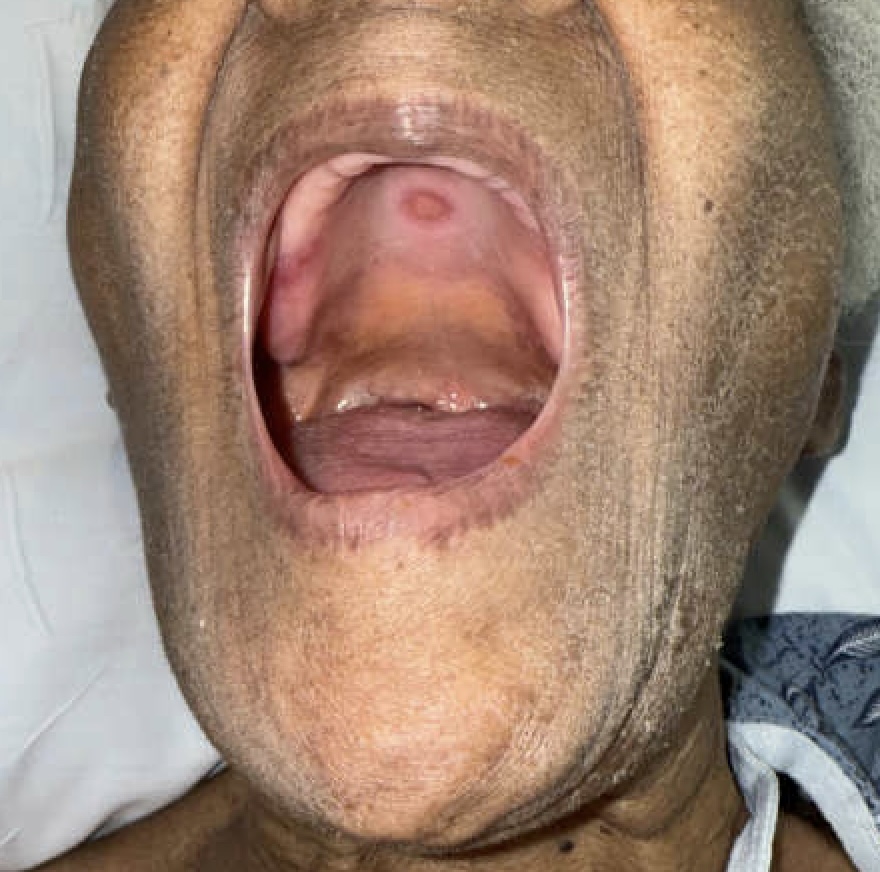
Discussion: Elderly patients are vulnerable to polypharmacy related dosing errors, including unintentional overdose of weekly medications. MTX, when taken more frequently than prescribed, can cause myelosuppression, mucositis (Figure), hepatotoxicity, and encephalopathy (1). In this case, daily MTX ingestion likely triggered early toxicity leading to encephalopathy, poor intake, dehydration, and AKI, which further impaired MTX clearance. Oral MTX is about 50 percent protein bound and distributes to extravascular compartments (2). Serum MTX levels are often low or undetectable at presentation and should not be used to exclude toxicity; toxicity has been reported despite normal levels (3). For low dose MTX in RA, routine level monitoring is not recommended. Management should be guided by symptoms, cytopenias, and mucositis (4). Our patient did not require IV leucovorin because cytopenias improved rapidly with oral folic acid. In a randomized trial, high and low dose leucovorin produced no difference in 30-day mortality or recovery time (5). Morbidity and mortality in severe low dose MTX toxicity are driven chiefly by complications of profound cytopenias, particularly sepsis (6).
Conclusions: Early recognition of low dose MTX toxicity is essential and relies on clinical findings rather than serum levels, which are often low or undetectable at the time of toxicity. Accurate medication reconciliation is critical for weekly drugs prone to dosing errors. Awareness of interacting agents such as Bactrim and close monitoring for mucositis, cytopenias, and renal dysfunction can prevent progression of toxicity. Supportive care with oral folate repletion is first line, while leucovorin is reserved for patients without early improvement in their cytopenias. Outcomes depend on preservation of functional progenitor cells, as folate supplementation can reverse toxicity only when the marrow is not fully ablated. Clinicians should remain vigilant for infectious complications, as sepsis rather than MTX toxicity itself, is often the principal driver of morbidity and mortality.