Background: BackgroundThe hospital environment is very often conducive to poor sleep. Factors contributing to this include environmental distractions such as noise and bright lighting, medical interventions, pain and anxiety.Studies of poor sleep in the general population suggest adverse effects on cognition, immune function, anxiety and pain.
Methods: MethodsThe DRĒMS study was conducted between Feb 2025 and July 2025 and included patients on two separate general medical floors of the hospital. The study consisted of an intervention and a control group with each group located on a different floor. All patients were adults who met the same inclusion criteria. Both groups had the same daily sleep questionnaires administered but no sleep interventions were utilized in the control group.In the study group, a multicomponent intervention was utilized. It consisted of a nighttime, nurse- driven sleep bundle which included:• Room lighting and temperature adjustment• Sleep and/or pain medications as needed• Toileting assistance• Offering blankets, sleep masks, ear plugs and a white noise generator• Reminding patients of call bell availability• Patients’ room doors were left open or closed on requestNurses were instructed to sign off in a log book to monitor for sleep bundle compliance.Additional interventions:• Room computer monitors were programmed to display a dark screen at night.• Nighttime nurse huddles to help minimize room interventions• Protocols to minimize unnecessary nighttime phlebotomies and daily weights• Protocols to decrease unnecessary telemetry monitoring• Sleep study signage was prominently displayed at the front of the medical ward and on all patients’ room doors. • Progress charts of patients’ sleep scores were prominently displayed for nurse viewing to help promote positive motivation with the study.A brief, daily sleep study was conducted by trained Patient Attendant Safety Aides who recorded both patient’s subjective sleep responses as well as any factors the patient felt affected their sleep. These questionnaires were reviewed by the floor nursing supervisor in real-time. When possible, additional appropriate interventions were then made to help with a patient’s ongoing sleep problem.
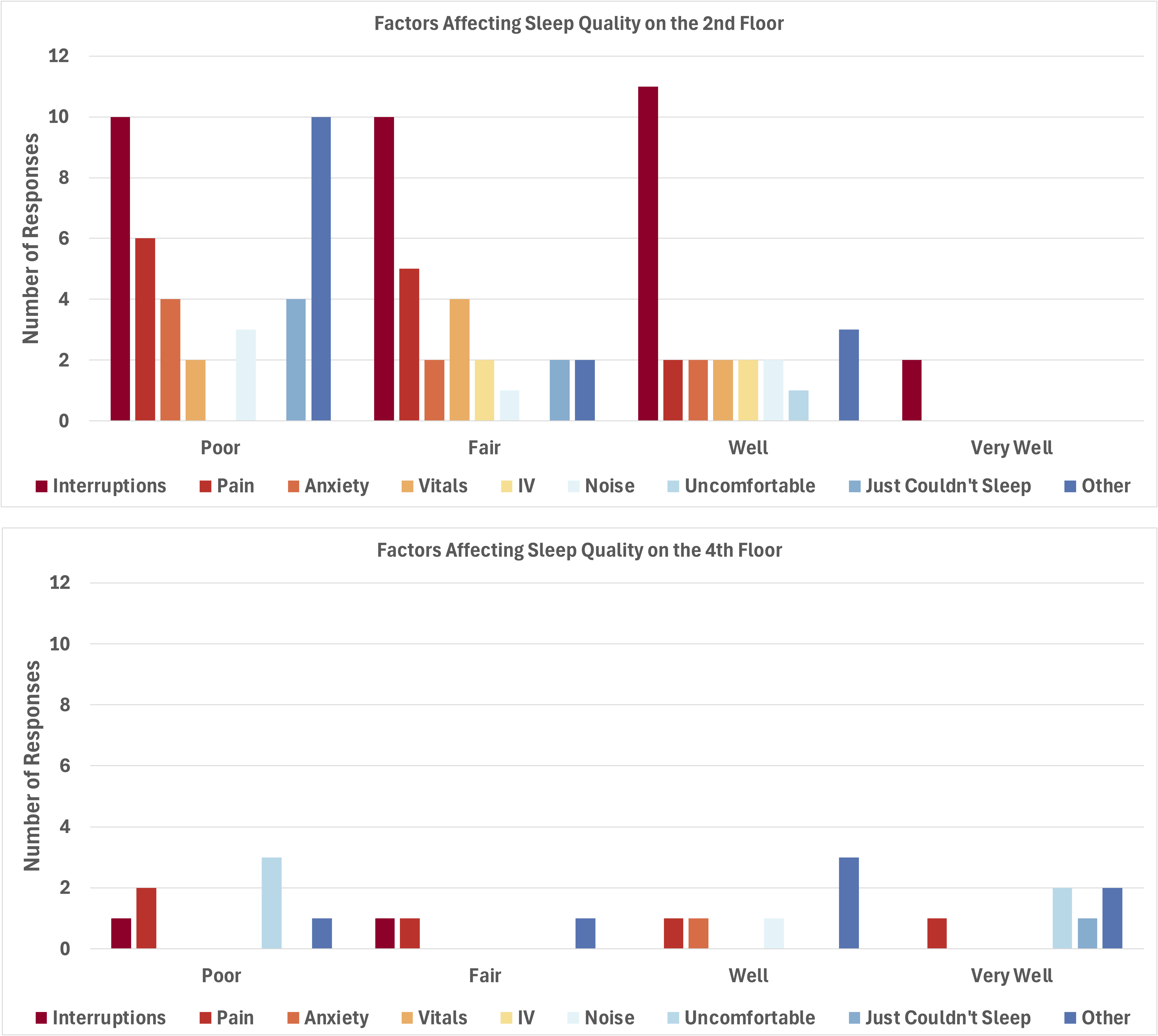
Results: ResultsData from 152 patients were analyzed. There were 83 patients in the intervention group and 69 patients in the control group. Comparing the intervention to the control group, the intervention group scored 26% higher in the combined slept well and very well grouping while the control group scored 26% higher in the slept poorly and fair combined groups. In the write-in comments section in the daily surveys which asked patients to simply report any factors they felt may have interfered with their sleep, the control group reported 409% more sleep related concerns compared with the intervention group. Sleep related concerns that were mentioned included sleep interruptions, pain, anxiety, being disturbed by the taking of vital signs, IV noises, environmental noises and being uncomfortable.
Conclusions: Conclusion This study highlights the effectiveness of using multiple, simultaneous interventions to enhance sleep management for hospital patients. It also utilizes a novel, ongoing, monitoring and data analysis system to ensure high quality continuity of in-hospital sleep interventions over time.
.png)