Case Presentation: A 37-year-old African American female with history of colitis presented with dyspnea and cough. Workup revealed a pleural-based left upper lobe mass and mediastinal lymphadenopathy. She denied exposure to mold, fungus, chemicals, inhalants, farms, or birds. Pathology was inconclusive but revealed poorly differentiated granulomas. She was given a diagnosis of sarcoidosis (without associated uveitis, cardiac, or skin lesions) and treated with corticosteroids. Subsequent imaging showed resolution of the lung mass and she was tapered off steroids.
Two years after initial presentation, she presented with fever and one-month of abdominal pain, diarrhea, night sweats, and significant weight loss. CT scan showed diffuse intraabdominal abscesses. She received broad-spectrum antibiotics and underwent an exploratory laparotomy with splenectomy, partial pancreatectomy, cholecystectomy, and appendectomy. All infectious workup (including intraoperative bacterial, fungal, and acid-fast bacilli tissue cultures and amoeba antibody) returned negative and pathology showed multifocal fibrinopurulent abscesses. Colonoscopy demonstrated nodular ileal mucosa and aphthous ulcers in the terminal ileum.
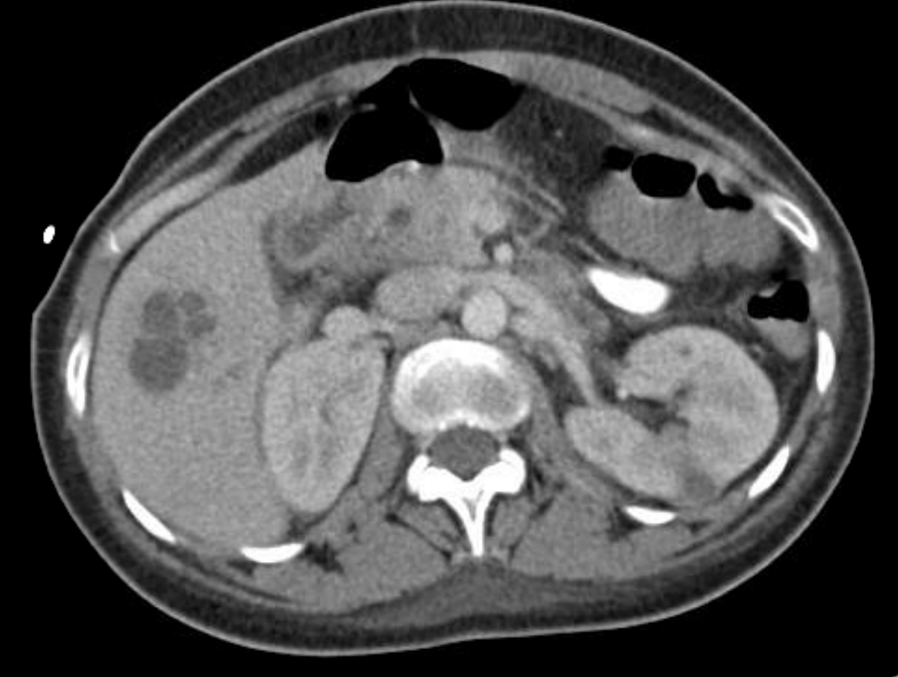
Eight months later, she presented with similar symptoms and was found to have multiple thick-walled liver abscesses. The patient underwent percutaneous drainage and again, all cultures were negative. She continued to have fevers to 103 despite antibiotics, although she was not toxic appearing. Labs were remarkable for ANA>1:2560, ESR>120, CRP 12.3, elevated proteinase 3 antibody, and normal complement and ACE levels.
Discussion: The recurrent nature of this patient’s presentation points towards a complication of an underlying process such as an autoimmune rather than infectious etiology. SAS consists of sterile collections of polymorphonuclear neutrophils in the absence of infection and has been associated with both IBD and relapsing polychondritis. Thus, this patient’s multiple “aseptic abscesses” and history of colitis were thought to be consistent with complicated IBD. A literature review shows that 94% of patients respond to corticosteroids, which suggests it is an effective first line therapy. This patient experienced rapid resolution of fevers and dramatic improvement with corticosteroids, further supporting this diagnosis. Recurrence rates of SAS may be up to 50%, however patients treated with maintenance therapy (i.e. azathioprine, sulfasalazine, adalimumab, or infliximab) typically do not have relapsing events compared to those on corticosteroids alone. Gastroenterology plans to start this patient on maintenance therapy at outpatient follow-up.
Conclusions: Sterile abscess syndrome (SAS) is a rare extra-intestinal manifestation of inflammatory bowel disease (IBD) with fewer than 50 cases reported to date. As seen with this patient, diagnosing and managing SAS can be challenging due to its atypical presentation.