Case Presentation: Many patients are being treated with biologic therapies for autoimmune diseases in the outpatient setting. It is critical for the hospitalist to recognize these patients as immunosuppressed and generate a broad differential when they are admitted to the hospital. The patient in this case was a 35-year-old male with a past medical history of Crohn’s disease on infliximab, hypogonadism on testosterone injections, hypertension, and anxiety/depression, presenting with a one-month history of progressively worsening headaches. The patient had actually been seen in the same emergency department prior to this presentation for headaches and sensory disturbances. CTA head and neck and MRI brain at that time both showed no acute intracranial abnormality. He was thought to have complex migraines and was referred to outpatient neurology. However, he re-presented days later due to erratic behaviors and labile personality changes in the context of persistent headaches.
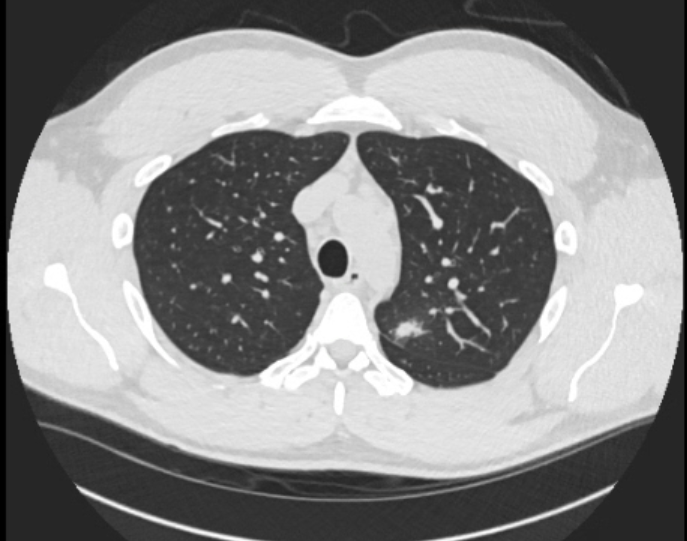
Discussion: He was somnolent in the ED, but otherwise, the initial vitals and physical exam were unremarkable. His urine drug screen was positive for amphetamines, barbiturates, benzodiazepines, and THC. CRP was mildly elevated to 8.7. No leukocytosis was noted. Given the recent negative CTA and MRI, a CTV was performed, which showed a flattened pituitary. Ophthalmology was engaged and noted grade 2 disc edema bilaterally. A lumbar puncture was performed with an opening pressure of 42, CSF protein of 76, normal glucose, 12 nucleated cells with 86% lymphocytes, and a negative meningitis/encephalitis panel. Serum/CSF cryptococcal antigen was negative. Autoimmune, paraneoplastic, and other infectious antibody panels were sent. He was initially diagnosed with idiopathic intracranial hypertension (IIH). Despite not being the typical demographic for IIH, his testosterone use and elevated BMI were posed as potential risk factors for IIH. Polypharmacy was also thought to be a contributor due to headache analgesics and other supplements. He was treated with acetazolamide with partial improvement in his headaches and mood. Six days after his admission LP, however, CSF Blastomyces antibody resulted strongly positive. A CT chest was obtained to look for disseminated disease: this revealed adenopathy and a micronodular pattern consistent with pulmonary blastomycosis. He was started on amphotericin.
Conclusions: This was a somewhat atypical presentation of fungal meningitis with many other competing differentials. Given the clinical context, IIH was felt to be a more plausible explanation initially despite a few pieces of primary data independently concerning for infection. When patients improve on initial therapy, it is tempting to anchor on the diagnosis, but this case highlights the critical importance of following through with a broad workup even if a working diagnosis has already been made. In the age of prevalent biologic therapy—especially TNF-alpha inhibitors—infectious etiologies must remain high on the differential.