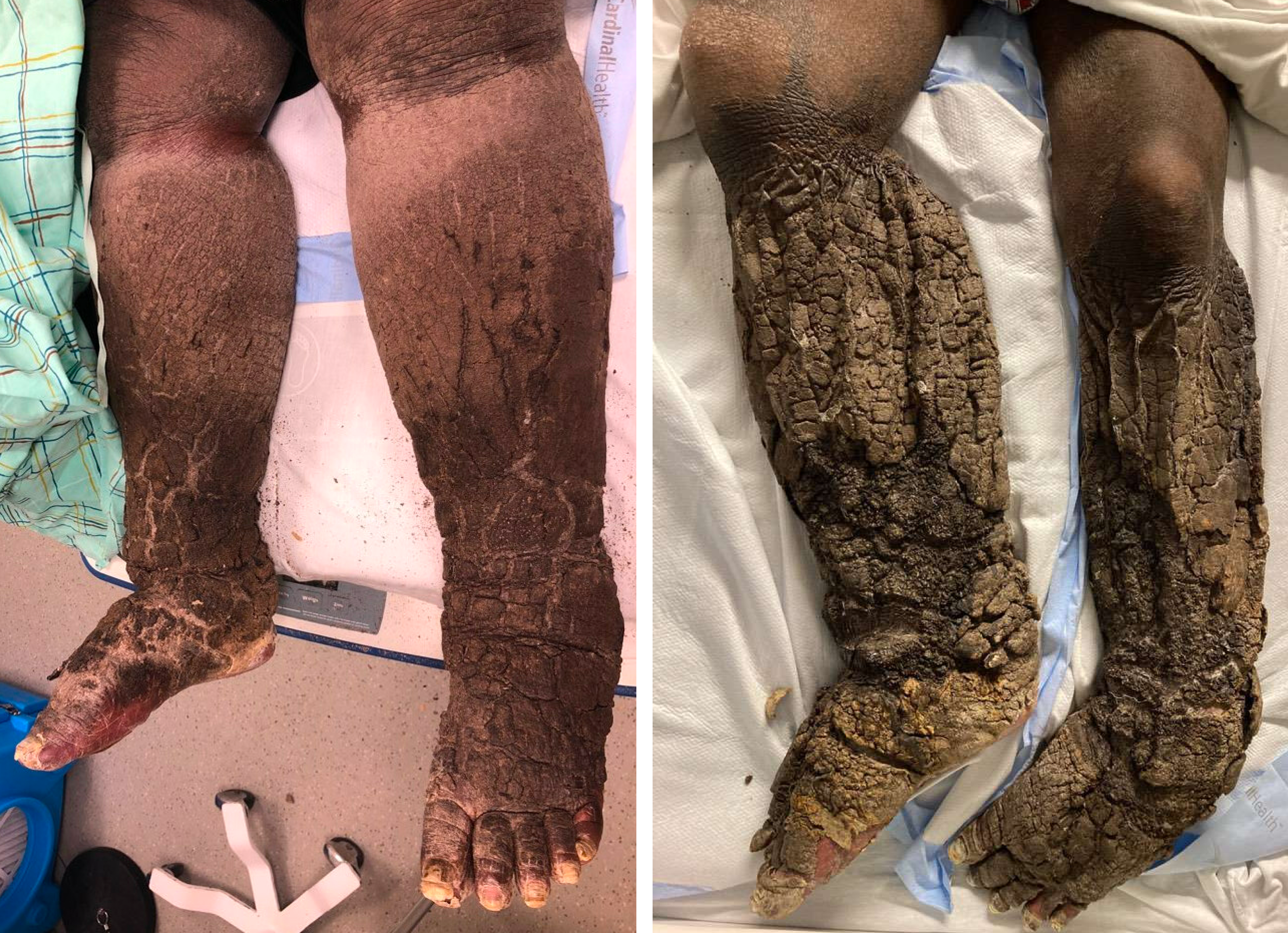
Case Presentation: A 56-year-old man with elephantiasis nostras verrucosa (ENV) was admitted to the hospital for fevers due to sepsis from lower extremity cellulitis. On exam, he was febrile to 102.1°F with HR 98 and BP 103/65. Cardiopulmonary exam was unremarkable. Malodorous indurated 2cm-thick brown plaques, embedded with gray and yellow debris, covered his feet and lower legs bilaterally (Fig. 1 & 2). Kaposi-Stemmer sign was present. He had pain with leg motion and debridement attempts. Labs showed WBC 15 x 10*3/uL, Cr 1.77mg/dL (was 0.84mg/dL), CRP 140.54mg/L, A1c 6.7%, and negative HIV serology. On CT scan, extensive bilateral subcutaneous fat stranding suggested cellulitis or subcutaneous edema. There was no evidence of osteomyelitis or abscess on MRI.On further history-taking, the patient reported that he was diagnosed last year with lymphedema and ENV. He was bedbound and had inadequate assistance with bathing and toileting. He did not adhere to mupirocin, manual lymphatic drainage, or recommended lifestyle changes, e.g. leg elevation at night. He denied sick contacts, travel, drug use, STDs, or filth or pests in his home.Based on the social history and exam compared to prior photographs, we diagnosed our patient with retention hyperkeratosis exacerbating ENV. Skin biopsy was avoided. The patient was managed with leg elevation, diuresis, ammonium lactate 12% lotion, and a course of IV Unasyn, leading to slow improvement in his skin lesions. However, limited mobility persisted, and his course was complicated by pulmonary embolism on hospital day 6, requiring escalation of care to the MICU.
Discussion: The differential for hyperkeratotic plaques on the legs is broad. Given our patient’s physical and social disabilities, we diagnosed severe retention hyperkeratosis from chronic inadequate hygiene. In this condition, also called dermatosis neglecta, the stratum corneum sheds insufficiently, mixing with sebum, sweat, and debris to form indurated plaques.We considered epidermodysplasia verruciformis, an autosomal recessive warty condition from HPV. But while HPV-unvaccinated, he was immunocompetent without related family history. Ichthyosis vulgaris also causes keratinization but spans a wider skin area with a “fish scale” appearance. Acanthosis nigricans was unlikely due to the location and good A1c control. Terra firma-forme dermatosis was ruled out given inefficacy of topical isopropyl alcohol.Our patient’s retention hyperkeratosis was thought to be an exacerbation of his existing ENV. ENV is a complication of chronic lymphedema when blocked lymphatic ducts cause fluid to collect in the dermis and subcutaneous tissues, leading to woody hypertrophic and verrucous skin changes. The patient had difficulty with self-care, medication use, and efforts to reduce venous stasis, leading to worsening of his edema and hyperkeratosis. A thorough social history, skin exam, and availability of comparison photographs differentiated between prior ENV findings and current overlying retention hyperkeratosis.
Conclusions: Recognizing retention hyperkeratosis helps to discern patients unable to care for themselves in difficult social circumstances. Unnecessary skin biopsy can be avoided with a detailed social history and photographic documentation in the medical chart. Although a dermatologically benign disorder, retention hyperkeratosis can seriously impact quality of life when unidentified and untreated. Resulting immobility increases risk for infection and hypercoagulable complications.