Background: Interdisciplinary rounds are widely recommended to improve communication, reduce care fragmentation, and enhance discharge efficiency. However, their effectiveness varies depending on structure, workflow alignment, and discipline engagement. In 2024, our health system implemented a standardized Structured Interdisciplinary Rounds (POCR) model across few inpatient medical units. The model included a structured script, a unified flow board, and defined roles for nursing, case management, pharmacy, and providers. We sought to evaluate early perceptions of the intervention across disciplines.
Methods: A quantitative Likert-scale survey was distributed to all rounding participants (providers, nursing, pharmacy, case management) one year after implementation. Responses were captured anonymously using Microsoft Forms and analyzed in Excel and R. Items were grouped into thematic domains: Nursing Workflow Support (6 items), Pharmacy Engagement (6 items), Case Management Coordination (5 items), Communication & Collaboration (4 items), Role Clarity & Efficiency (4 items), Patient Impact & Safety (3 items), and Operational Friction (1 item). Scores were converted to a 1–5 scale (1=Strongly Disagree; 5=Strongly Agree). Favorability was defined as responses ≥4. Descriptive statistics were generated for each domain.
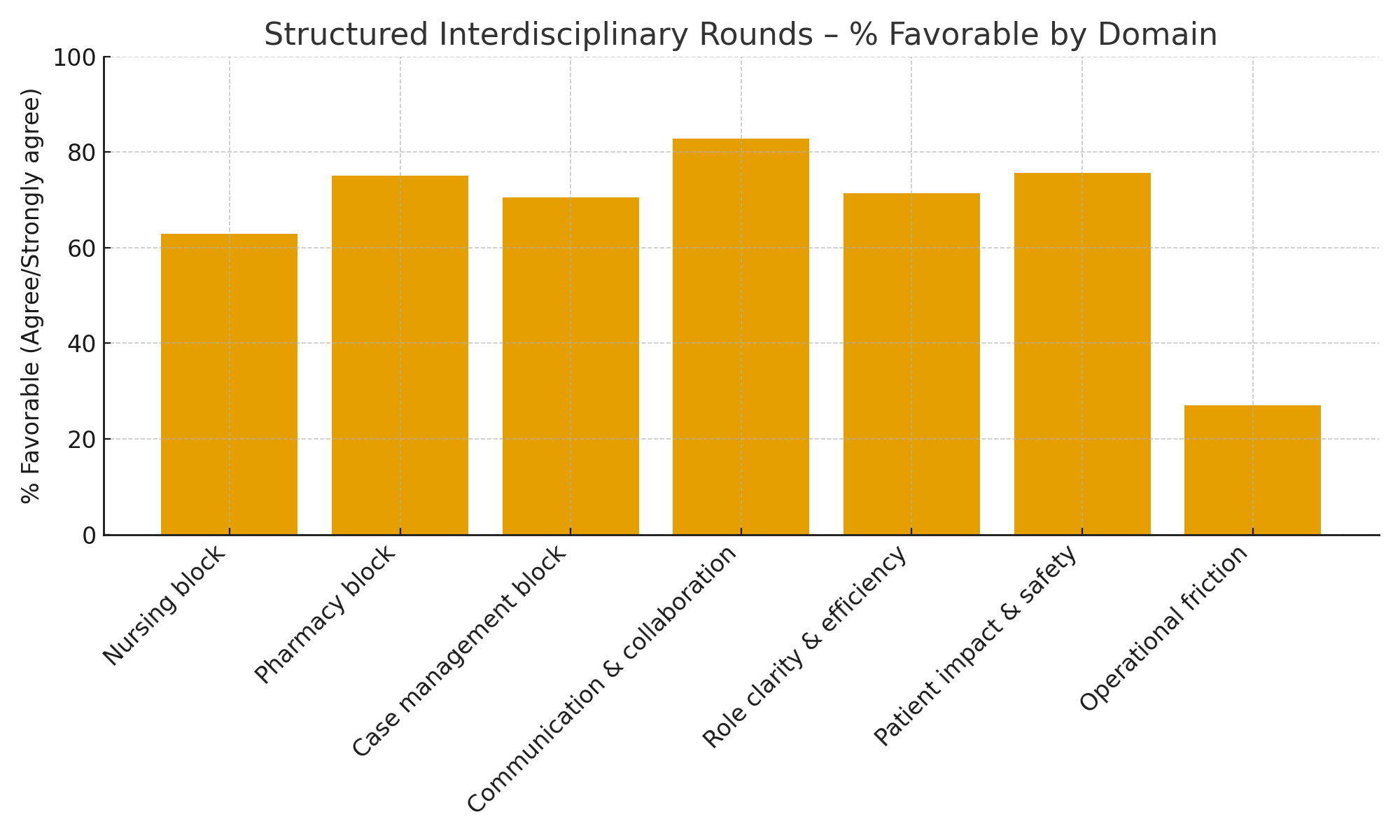
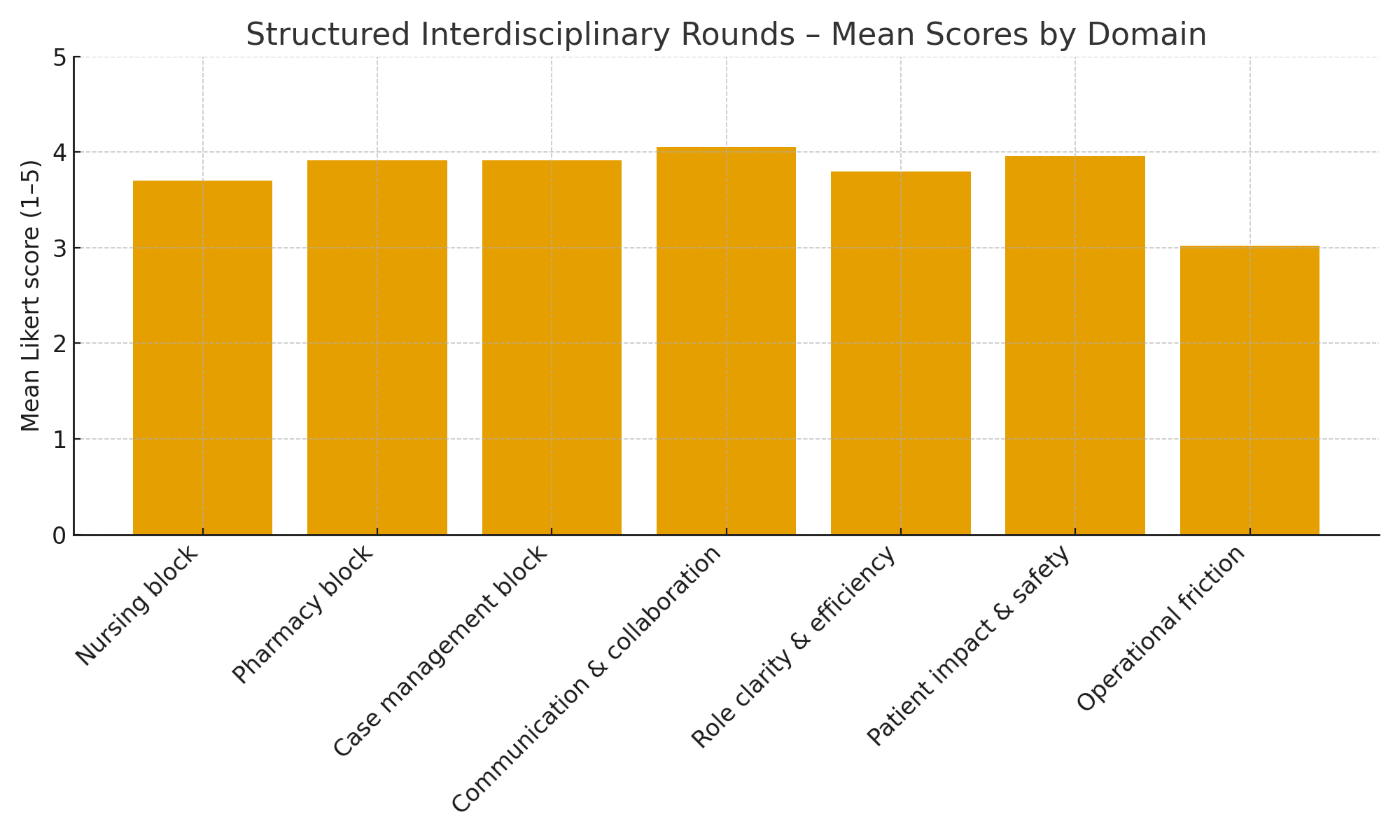
Results: A total of 48 full responses were analyzed. The Communication & Collaboration domain scored highest (Mean 4.05; 83% favorable), indicating strong improvement in shared plans of care, reduction in miscommunication, and perceived team alignment. Patient Impact & Safety showed similar strength (Mean 3.96; 76% favorable), with respondents noting improved timeliness of interventions and earlier identification of discharge barriers. Case Management Coordination performed well (Mean 3.92; 71% favorable), especially for clarity in discharge readiness (94% favorable).Nursing Workflow Support showed moderate gains (Mean 3.70; 63% favorable), with opportunities to improve timely provider orders and reduce the need to chase updates. Pharmacy Engagement also trended positive (Mean 3.92; 75% favorable), though limited by small sample size (n=12 item-level responses).The primary area of concern was Operational Friction: “Too many participants make rounds inefficient” scored lowest (Mean 3.02; 27% favorable), indicating perceived crowding and workflow disruption.
Conclusions: Evaluation of POCR demonstrates strong improvements in communication, shared decision making, discharge clarity, and patient-safety-related coordination. However, efficiency benefits remain mixed, with consistent feedback about participant volume and bottlenecks in timely order placement and equipment/transport coordination. These findings suggest that structured interdisciplinary rounds are most effective when paired with clearer role assignments, streamlined participant presence, and rapid-order pathways for items arising during rounds.