Background: Healthcare has become exponentially more complex with intricate systems of care delivery and large, diverse, subspecialized provider teams. Because of the multi-faceted nature and promise of effective leadership, many healthcare systems have turned to leadership development as a strategy to address the challenges this complexity brings. Leadership development programs have historically targeted traditional hierarchical leaders, those targeted as individuals with leadership potential, or specific homogeneous groups of individuals such as internal medicine residents. In this context, the Medicine Service at the VA Ann Arbor created and implemented Fueling Leadership in Yourself (FLY), a novel faculty and staff development program.
Purpose: To engage all levels of healthcare providers in leadership development activities in an effort to invigorate a collaborative culture, elevate faculty and staff autonomy, enhance employee satisfaction, and improve quality of care.
Description: Between April 2017 and June 2018, two series of leadership development sessions were facilitated by VA Ann Arbor leaders including series creators and content expert guest speakers. Each series contained 4 one-hour sessions from 12:00pm to 1:00pm that occurred monthly. Email invitations were distributed to all faculty and staff within the Medicine Service, regardless of professional role. Content areas focused on leadership approaches and attributes that are applicable to all roles within a healthcare system. These included the art and science of leadership, empowering mindfulness techniques in the workplace, quality improvement strategies in daily work, and effective communication principles.
Sessions were intentionally spaced apart monthly and embedded during a typical lunch break to ensure maximal participation with minimal disruption to clinical care. Catered meals were provided at each session. A variety of teaching methods was employed including think-pair-share discussions and group reflections, video explanations of key concepts, mindfulness exercises, group exploration of the patient journey to identify opportunities for small tests of change, and interactive improvisational exercises to elevate communication skills.
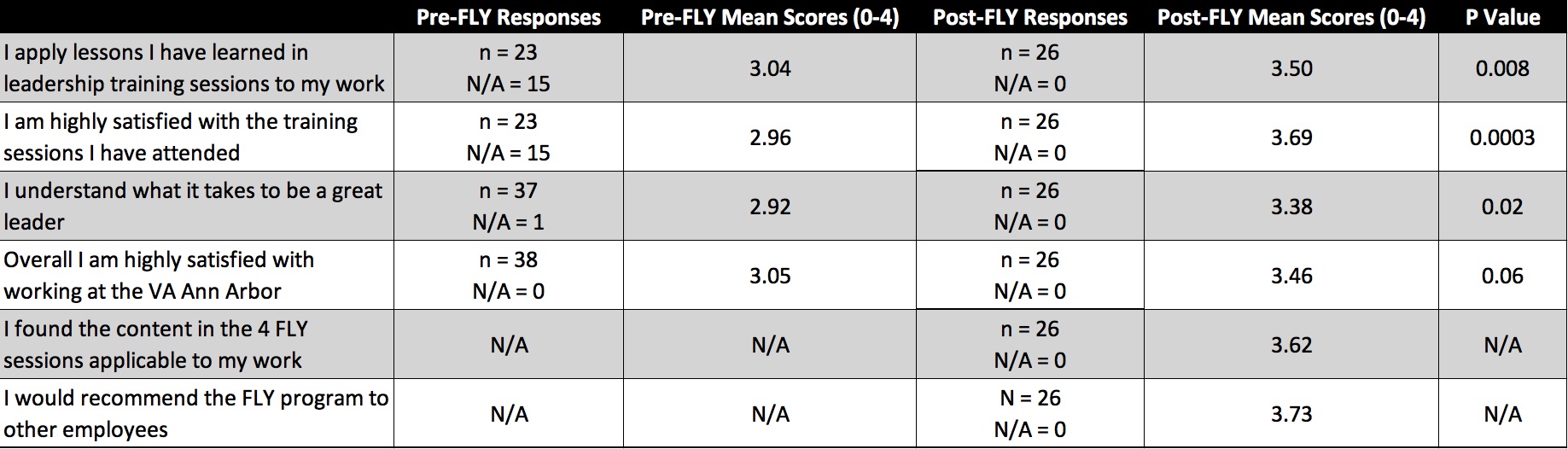
Surveys were collected before the first session and following the fourth session in an effort to understand the series’ quality and impacts. These surveys elicited Likert scale responses from participants (Table). Of 38 participants from 8 distinct departments, all 38 (100%) completed the pre-series survey, and 26 (68.4%) completed the post-series survey. For all responses, “0” indicated strongly disagree, “2” indicated neither disagree nor agree, “4” indicated strongly agree, and “N/A” indicated not applicable. A numeric value was assigned to each answer from 0-4, and means were calculated. All ‘N/A’ answers were deducted from data analysis.
Conclusions: FLY participants from multiple departments and different roles were highly satisfied with the leadership training sessions and showed an improvement in satisfaction with working at VA Ann Arbor. Expansion of the series to other services is planned.