Background: Hospitalists are core to the U.S. inpatient provider workforce and serve a central role in adults’ inpatient health system interactions. Over 11 million Americans identify as lesbian, gay, bisexual, transgender, or queer (LGBTQ) [1] and 1 in 6 LGBTQ Americans describe facing discrimination in the medical setting [2]. To provide culturally responsive and clinically competent care, hospitalists must understand the specific social and health needs of LGBTQ patients. We developed the Q-HEALTH survey to identify hospitalists’ attitudes and knowledge around LGBTQ health, and to guide future educational interventions.
Methods: After IRB review, the Society of Hospitalist Medicine (SHM) LGBTQ health education working group formed a 58-question Qualtrics survey, and emailed requests for anonymous participation through the SHM members’ listservs (January – June 2019).
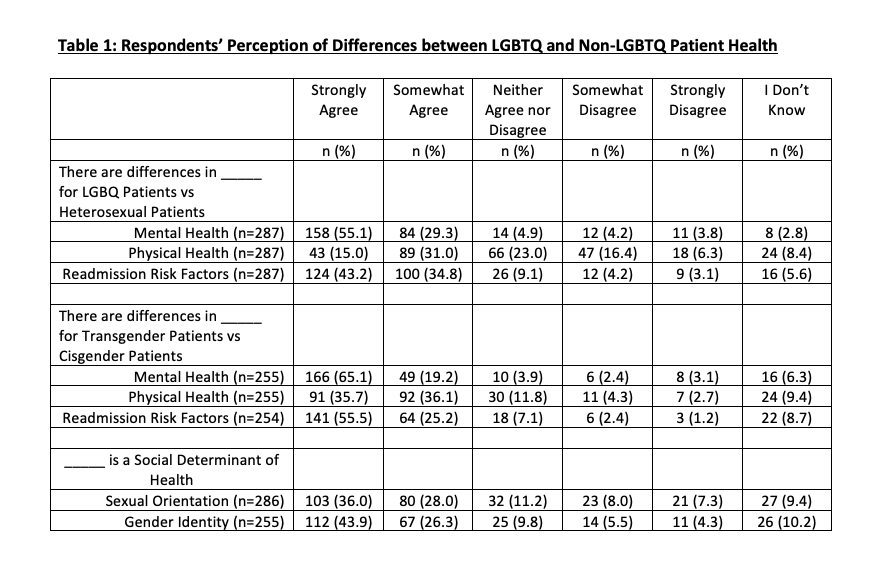
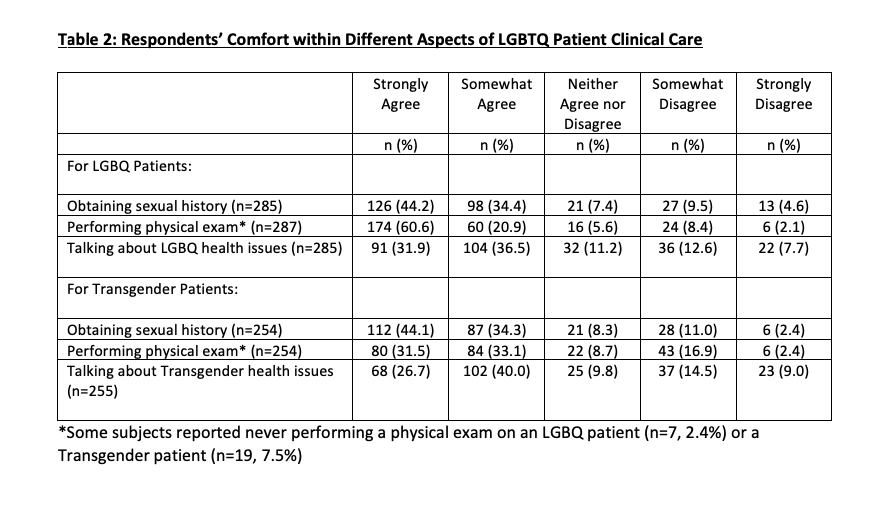
Results: A total of 456 respondents started and 238 finished the survey (Female/Male/Non-binary: 59%/38%/2%). Twenty percent identified as lesbian, gay, bisexual, or queer (LGBQ). Respondents had MD/DO (78%) or NP/PA-C (22%) training, and were aware of working with LGBQ or transgender (T) patients more than once a year (LGBQ: 86%, T: 51%). 77% somewhat or strongly agreed to feeling comfortable explaining the difference between sexual orientation and gender identity. Many were comfortable working with LGBTQ patients “most of the time” or “always” (LGBQ: 91%; T: 78%), though fewer felt clinically competent (LGBQ: 72%; T: 51%). Respondents somewhat or strongly agreed to being as comfortable performing a physical exam on LGBQ patients compared to heterosexual patients (82%), though this number decreased for transgender patients compared to cisgender patients (65%). Many respondents somewhat or strongly agreed that LGBTQ individuals faced disparities in mental health (LGBQ: 84%; T: 84%), though fewer agreed about physical health disparities (LGBQ: 46%; T: 72%) or that LGBTQ identity was a social determinant of health (LGBQ: 64%, T: 70%). Only 29% correctly identified that bisexual individuals face worse health outcomes compared to their lesbian or gay peers [3]. 74% wanted further LGBTQ health training.
Conclusions: This is the first survey to specifically assess hospitalist LGBTQ health knowledge and attitudes nationally. Limitations include low sample size, and respondent self-selection bias. Responding hospitalists reported overall comfort, though less clinical competence, in working with LGBTQ patients. Many reported more familiarity with LGBQ health than Transgender health, and some were not very familiar with physical health disparities faced by the LGBQ population or with physical examination of the transgender patient. A majority favored more LGBTQ health education.