Background: The Physician Orders for Life-Sustaining Treatment (POLST) form is an important tool to elicit and document patients’ treatment preferences in a way that is valid across health care settings. Studies on its efficacy have found high rates of consistency between patients’ treatment preferences for cardiopulmonary resuscitation (CPR), medical interventions, and artificial nutrition documented on POLST forms with treatments patients receive. Over 80% of Californians believe that it is important to have discussions and documentation of their preferences for health care, yet only 23% have written documentation of their end of life wishes.
Purpose: To increase advanced care planning documentation using POLST forms among patients with a Do Not Resuscitate (DNR) or Partial Code order who are cared for by the Hospital Medicine Service at a large academic tertiary care hospital.
Description: In the academic year prior to our intervention, the average rate of the POLST completion for hospital medicine patients with a DNR or Partial Code order was 41%. To understand the barriers to more consistent POLST completion, we met with key stakeholders including hospitalists, palliative medicine physicians, social workers in hospital medicine and palliative care, and social work/case management leadership. We mapped the typical process for POLST completion, brain-stormed about common lesions in this process, and charted potential process changes on a prioritization chart. Common barriers identified included lack of awareness about POLST forms, low provider confidence in advanced care planning conversations and the completion of POLST forms, accessibility of POLST forms, and lack of accountability for POLST completion.
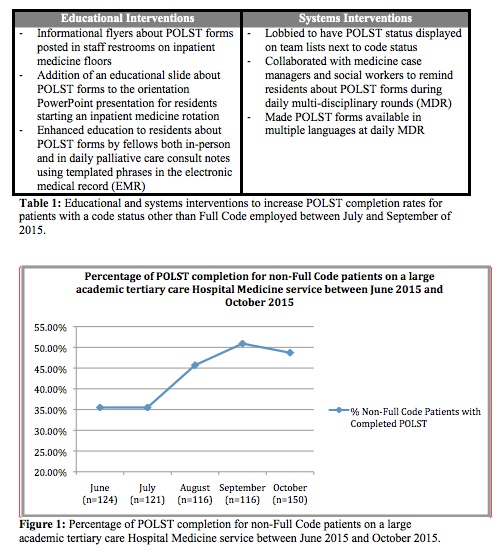
The palliative medicine fellows set a goal of increasing the rate of POLST form completion from 41% to 75% in at least 9 of the next 12 months for patients discharged from the Hospital Medicine Service with a code status other than Full Code. We used multiple interventions to drive change (Table 1). First quarter data show an increase in POLST completion rates for patients who are discharged from the hospital with a code status other than Full Code (Figure 1).
Conclusions: Targeted multi-modal educational and systems interventions can improve advance care planning documentation. Next steps include providing monthly feedback reports comparing individual medicine teams to the service overall to increase accountability, give positive reinforcement, and offer greater incentive for improvement.