Background: Point-of-care ultrasound (POCUS) is increasingly emphasized in undergraduate medical education (UME), with the expectation that Internal Medicine (IM) residents enter graduate medical training with greater POCUS knowledge. However, the impact of UME curricular changes on POCUS knowledge and confidence among IM residents is unclear. The objective of this study was to determine if matriculating IM residents demonstrate greater POCUS knowledge in 2025 than in 2019, hypothesizing that recent UME emphasis would result in higher POCUS knowledge.
Methods: Cross-sectional surveys were administered to IM residents at a single academic center in 2019 (N=78) and 2025 (N=25). The 2019 cohort included PGY1-3 residents prior to implementation of formal residency-based POCUS curriculum. The 2025 cohort included incoming PGY1 residents only. Surveys assessed demographics, prior POCUS training, POCUS confidence and perceptions, and knowledge in four domains: physics/probe use, procedural use, image acquisition, and image recognition. While survey content was iteratively refined, core questions were comparable. Confidence intervals were available for 2025 data but not for 2019. No formal statistical comparisons were performed due to survey modifications. Medical school data was collected to assess geographic and institutional diversity of participating residents.
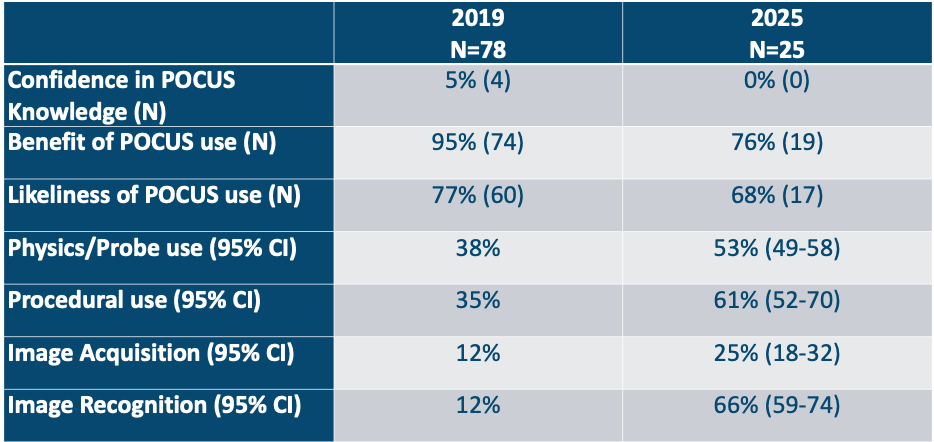
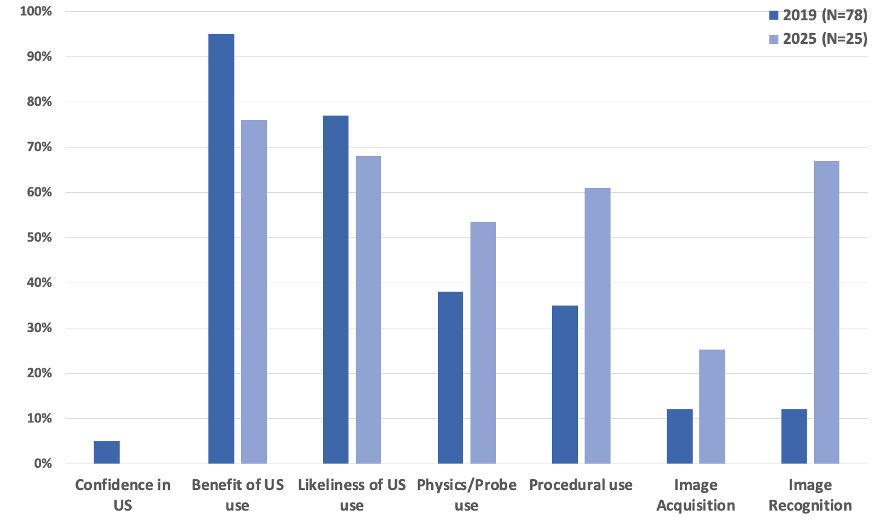
Results: Residents represented a wide range of US allopathic, osteopathic, and international medical schools, contributing to diversity in baseline POCUS exposure and perspectives. From 2019 to 2025, prior POCUS training increased 18% to 68%, yet POCUS confidence remained low (5% vs 0%). Perceived benefit of POCUS and likelihood to use were high both years but decreased in 2025 (benefit: 95% vs 76%; likelihood: 77% vs 68%). POCUS knowledge improved across all domains: physics/probe use (38% vs 54% [49-58%]), procedural use (35% vs 61% [52-70%]), image acquisition (12% vs 25% [18-32%]), and image recognition (12% vs. 67% [59-74%]).
Conclusions: Compared to 2019, incoming IM residents in 2025 had greater prior POCUS exposure and knowledge across all domains, consistent with increased UME curricular emphasis. However, self-reported POCUS confidence remains low, and perceived benefit and likelihood to use declined modestly. This discrepancy suggests that despite greater knowledge, hands-on experience and clinical integration may lag, highlighting the need for residency curricula to bridge the gap. Specifically, this divergence of perception and knowledge may closely trace the Dunning-Kruger effect and actually represent increasing knowledge with cognitive bias. Geographic and institutional diversity of residents underscores the importance of adaptable yet standardized POCUS training. Limitations include lack of direct statistical comparison and absence of 2019 confidence intervals. Future directions include standardized, longitudinal assessments and qualitative exploration of barriers to POCUS confidence and use. Curricular efforts should prioritize not only knowledge acquisition but also practical skill development to ensure increased knowledge translates to effective clinical application.