Background: Patient experience is increasingly recognized as a measure of healthcare quality and patient-centered care. However, there is insufficient understanding of patient expectations during hospitalization, and of how these are perceived by physicians, nurses, and administrators. The best way to apply the HCAHPS ratings remain elusive due to variability in practice environments, patient and clinician diversity and bias. The scores do not tell the full story and there have been recent calls to modify HCAHPS to better reflect shifts in patient experience in the last decade. Patient feedback regarding care experiences can be utilized in novel ways to improve the care experience. In this study, we aimed to 1) explore concepts identified by patients as being important to them during hospitalization, 2) explore concepts believed by physicians, nurses, and administrators to be important to patients during hospitalization, and 3) identify gaps and similarities between patient and healthcare professional perceptions and expectations.
Methods: We conducted a qualitative study at a university-affiliated, safety net hospital utilizing semi-structured interviews with hospitalized English- and Spanish-speaking patients and focus groups with physicians, nurses, and administrators. Interviews and focus groups were audio-recorded, transcribed verbatim, and analyzed using inductive thematic analysis.
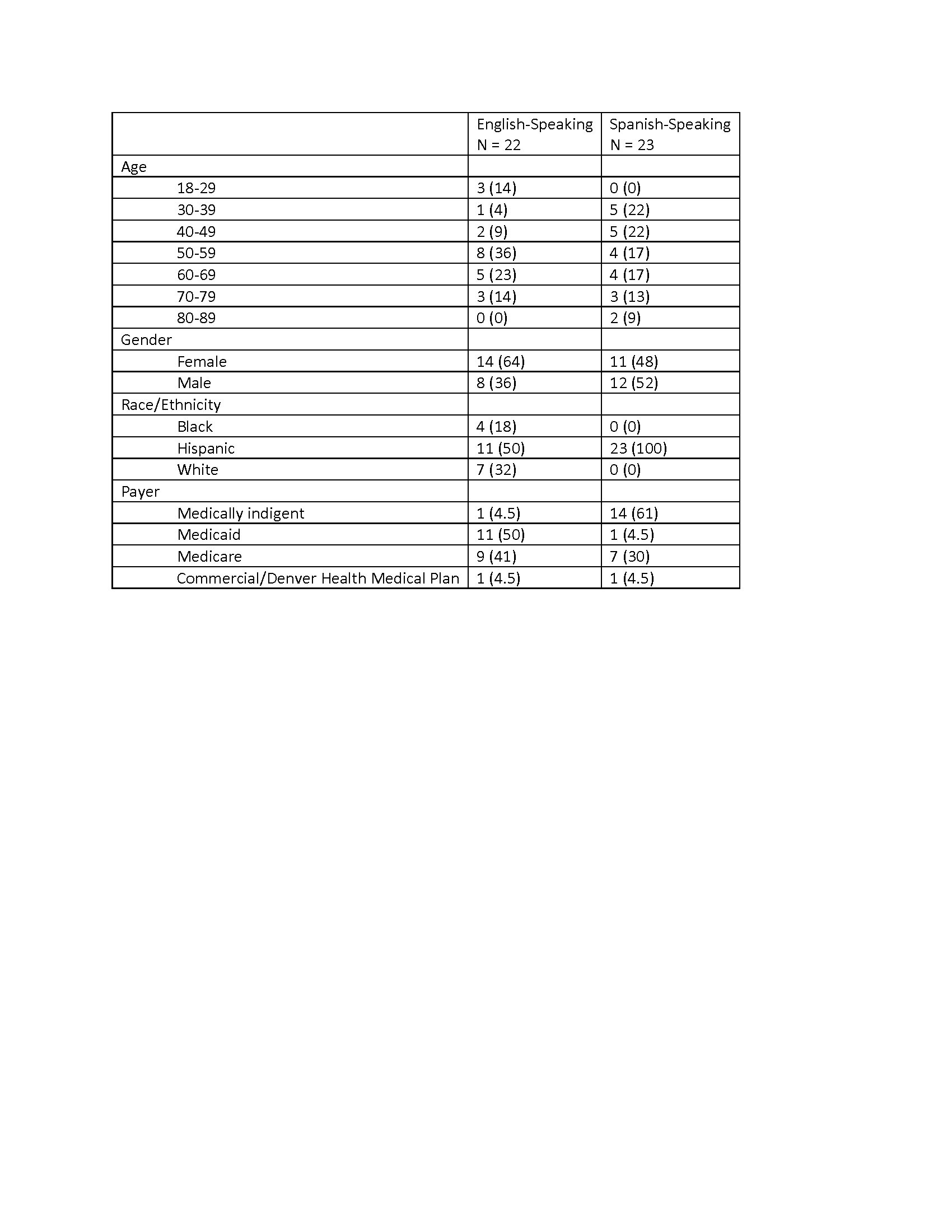
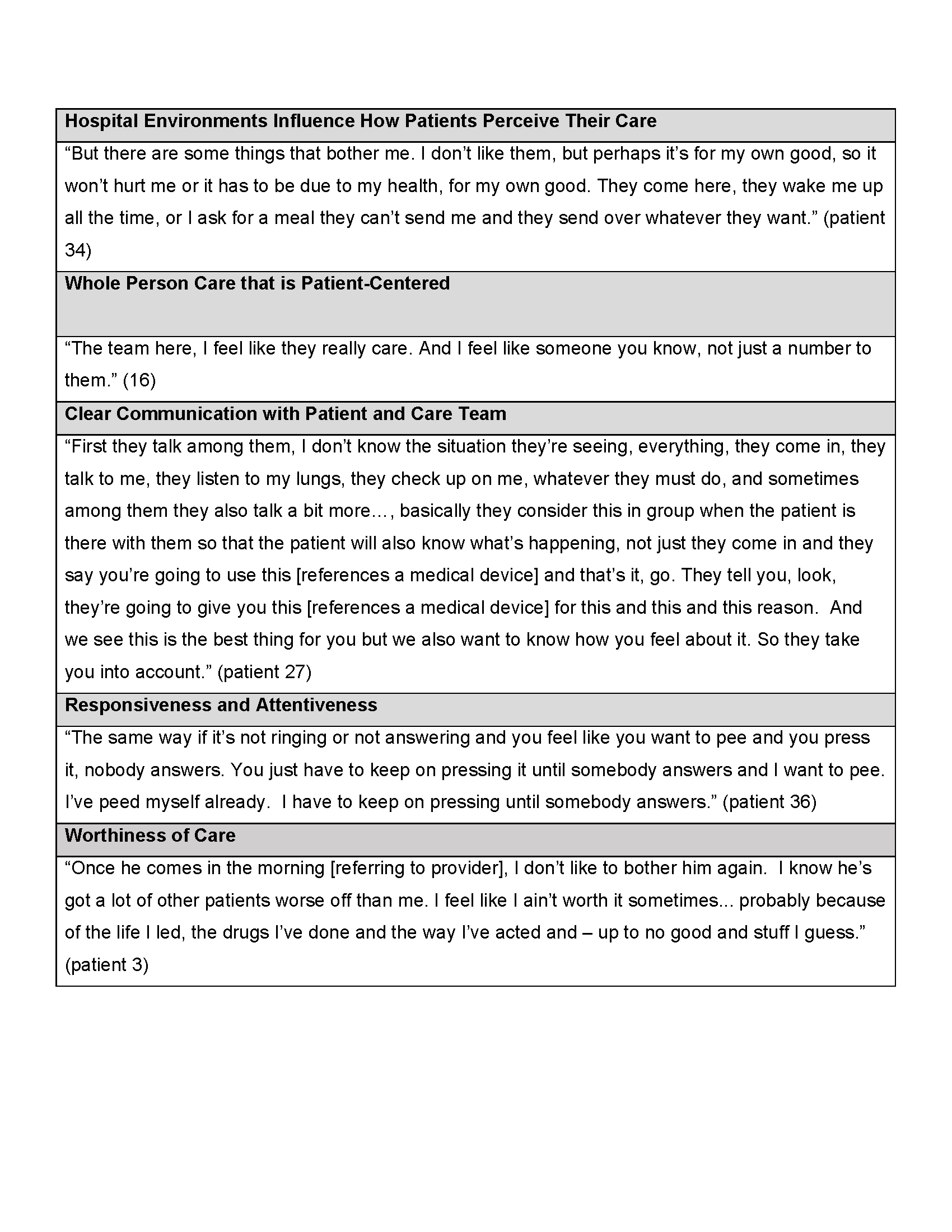
Results: Forty-five patients were interviewed and six focus groups were conducted with 13 physicians, 10 nursing staff, 15 managers, and seven executives from March 22, 2016 to May 15, 2017 (Table 1). The most important findings of this study are: 1) patients value whole person care, defined as holistic treatment that includes emotional and social needs along with treatment of illness, clear communication with their care providers, attentiveness and responsiveness to their needs, and a hospital environment that is conducive to healing (Table 2); 2) a sub-group of patients expressed the feeling of a lack of worthiness and a reluctance to self-advocate; 3) while physicians, nurses, and administrators can articulate what patients find most important, patients’ experiences indicate that hospitals struggle to bridge the gap between understanding patient needs and actually meeting those needs.
Conclusions: We found several critical themes among hospitalized patients, such as communication between care team members, not currently captured in standard patient experience assessments. We found that there is a disconnect between what patients and clinical staff believe patients need and want and what hospital policies and environments drive in the care environment. Certain vulnerable populations may be less inclined to self-advocate regarding their needs and additional measures may need to be taken to ensure needs are met.