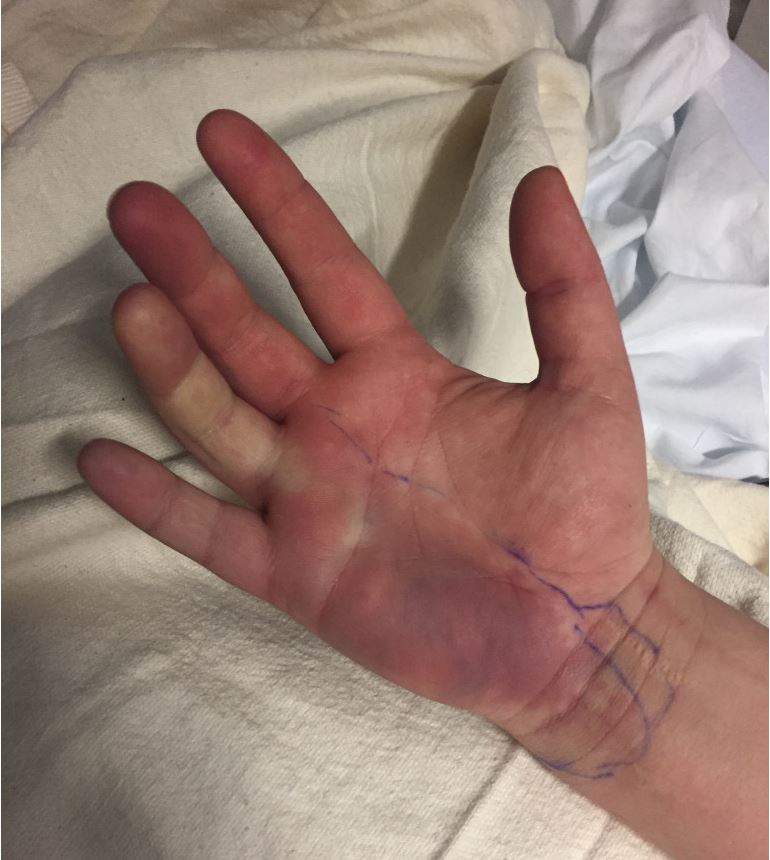
Case Presentation: A 25-year-old woman with a remote history of intravenous drug use, last reported seven months prior, presented with two days of progressive cyanosis and pain of the medial right hand with associated paresthesia, hyperesthesia, and stiffness. Physical exam revealed well-demarcated cyanosis of the fourth, fifth, and medial third digits extending to the wrist crease without ulceration; the area was cool to touch. Capillary refill was delayed; radial and ulnar pulses were palpable and equal bilaterally. Range of motion of the hand was limited by pain. Moderate edema without erythema was present. There were no murmurs or rashes appreciated.
Laboratory evaluation demonstrated normal ESR, CRP, lactate and white blood cell count. Blood cultures were negative. On CT angiogram, arterial vasculature of the right upper extremity was patent with an intact deep arch; vasculature distal to the arch was not well visualized. There were no valvular vegetations by transthoracic echocardiogram. Right upper extremity angiogram revealed complete focal occlusion of the distal ulnar artery extending into the palmar arch with collateral flow from the radial artery. She was started on a heparin drip but subsequently left against medical advice. She re-presented to a nearby facility three days later with symptom progression, at which time she reported injection of sublingual buprenorphine/naloxone into the right wrist the day prior to initial symptom onset.
Discussion: Amidst the opiod epidemic and the increasing use of opioid replacement therapy, the internist will encounter complications of substance abuse and misuse. When considering the differential of acute digital ischemia, one must review potential sources including septic emboli, autoimmune vasculitis, and hypercoagulability. A high index of suspicion must be maintained for particulate emboli, especially in patients with substance abuse history.
Buprenorphine/naloxone controls opiate cravings while minimizing withdrawal effects when administered sublingually. When dissolved in water, filtered, and injected, patients can obtain euphoria by diluting the naloxone component. Accidental arterial self-injection can lead to distal embolization due to the gelatinous component hydroxypropyl methylcellulose. This, along with injection-induced vasoconstriction and intimal blood vessel damage, leads to acute digital ischemia.
Upon diagnosis, intravenous heparin should be started promptly with ultimate transition to dual antiplatelet therapy. In most cases, tissue loss is unavoidable despite early detection and management. Patients must be warned of this potential complication when receiving sublingual opioid replacement therapy.
Conclusions: This case represents a rare but increasingly common complication of opioid replacement therapy amidst the current opiod crisis. With arterial injection, acute digital ischemia from hydroxypropyl methylcellulose emboli may arise. Prompt recognition and initiation of systemic anticoagulation can prevent progression of the ischemia but not ultimate tissue loss. Further efforts to prevent misuse and educate about this potential consequence must be undertaken.