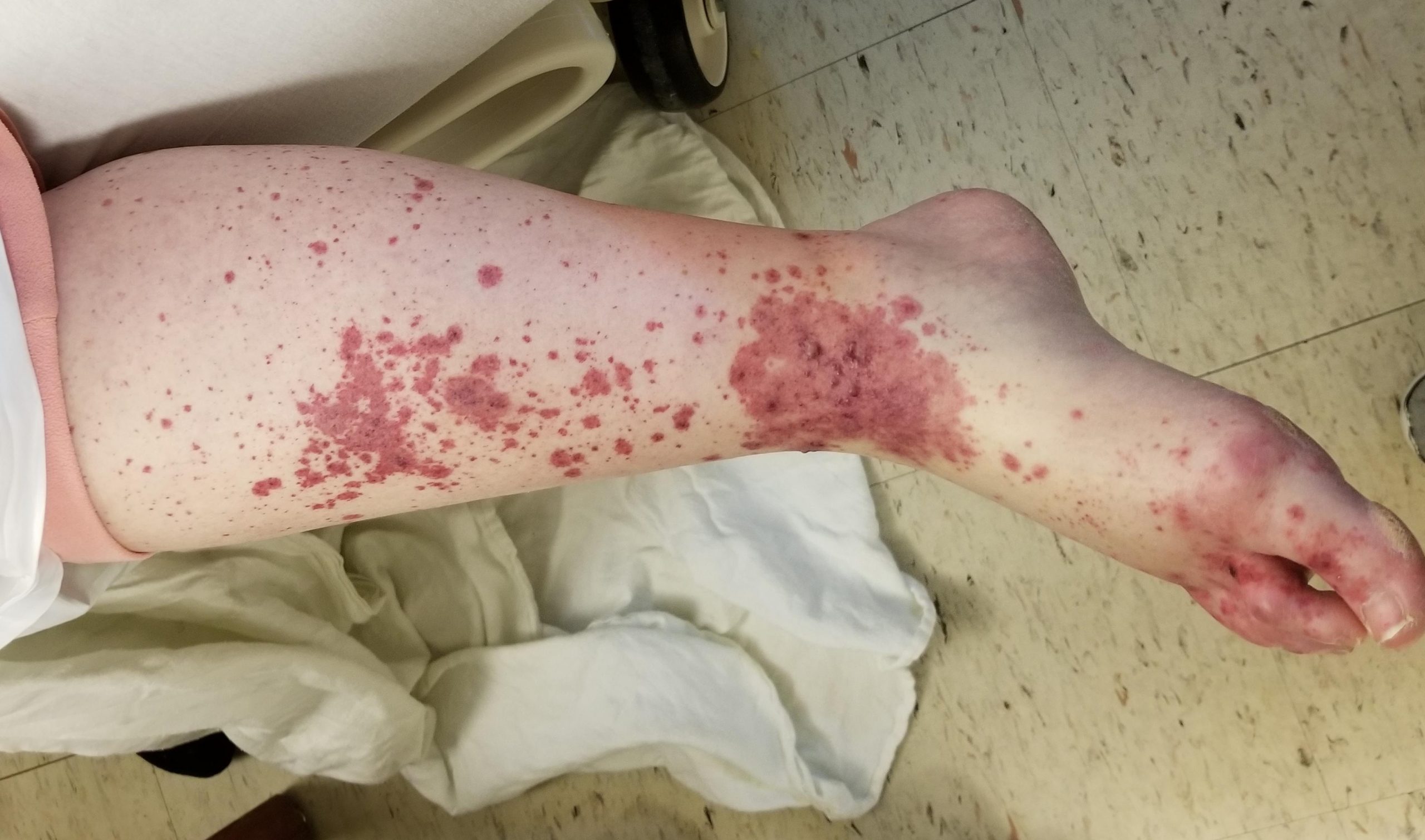
Case Presentation: 68-year-old white female presented with upper respiratory tract symptoms which progressed to cough in 4 days and she was found to have a right lower lobe pneumonia. Her sputum culture revealed MSSA (Methicillin Susceptible Staphylococcus Aureus) and she was treated with ceftriaxone and azithromycin. But her pneumonia worsened and she developed parapneumonic effusion, hence antibiotics were escalated to Vancomycin and piperacillin tazobactam. Within 2 days of antibiotics, patient developed violaceous confluent and tender palpable purpura entire body, more on bilateral lower extremities, consistent with a vasculitis. Piperacillin- tazobactam was discontinued and she was initiated on oral prednisone 20 mg daily . Simultaneously her renal function worsened and she developed hematuria, nephrotic range proteinuria, oliguric acute renal failure, hence oral steroid was changed to pulse dose steroids. Her serological work up was unremarkable with negative ANCA, negative Anti-GBM and normal complements. Kidney biopsy showed diffuse endocapillary proliferative and exudative immune-complex GN with a few crescents with mesangial predominant IgA deposition. Patients rash improved with steroids, but renal function worsened to 4.7 mg/dl on steroids and patient continued to be oliguric. She was started on hemodialysis(HD), which improved the clinical condition and she was able to come off after few sessions of HD. Currently she follows up with outpatient nephrology, has Stage 4 kidney disease with proteinuria.
Discussion: Post infectious glomerulonephritis is mostly used synonymously with post streptococcal GN. It still holds good for children, however in adults staphylococcal glomerulonephritis is the more common cause. Cutaneous vasculitis can occur in patients with staphylococcus-associated glomerulonephritis, imitating IgA vasculitis (Henoch-Schönlein Purpura) or antineutrophil cytoplasmic autoantibody (ANCA)-associated vasculitis. Treatment focus on eradicating the infection, relieving symptoms, and controlling hypertension and edema. We do not use immunosuppressive therapy in these patients, which might explain the progression of renal disease in our patient despite being on steroids.
Conclusions: Staphylococcal pneumonia is quite common cause of inpatient admission and patients with Staphylococcus-associated glomerulonephritis, particularly older adults , have a concurrent staphylococcal infection like our patient. .We presented a rare complication of staphylococcal pneumonia resulting in rapidly progressive glomerulonephritis (RPGN) and purpuric rash mimicking vasculitis. Prompt action and understanding this complication of Staphylococcal pneumonia will help us with early nephrology referral and HD.