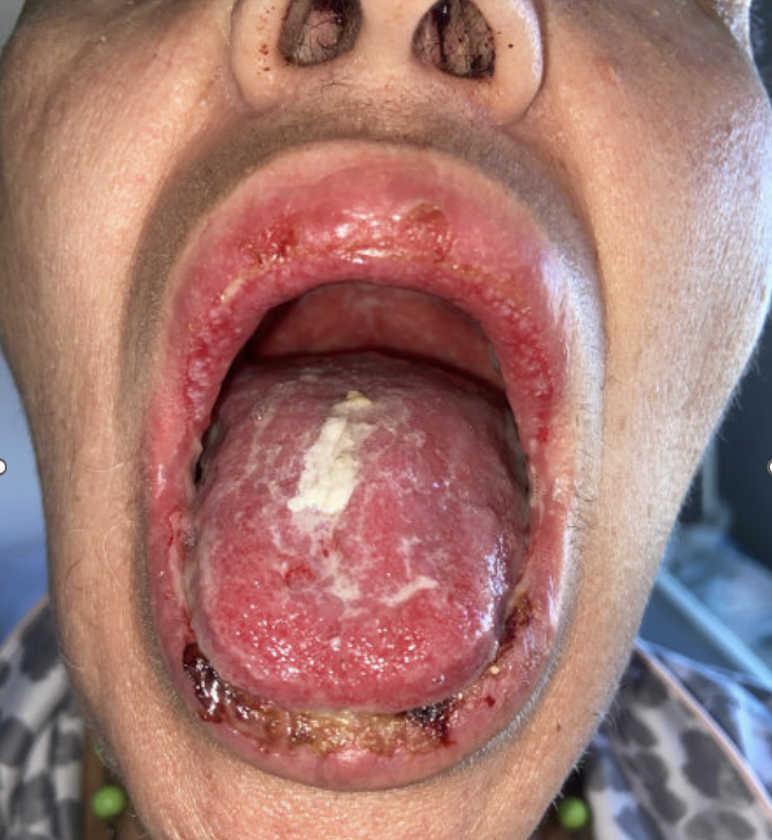
Case Presentation: A 61-year-old woman with no significant medical history presented with two months of progressive mucositis. A few days after routine dental radiographs two months prior, she developed severe odynophagia with extensive oral ulcerations. She was unable to tolerate oral intake and reported 17 lbs weight loss. Per report, she had tested positive for HSV-1 PCR one month prior. Outpatient treatments had included antibiotics (amoxicillin, clindamycin), acyclovir, fluconazole, and a two week course of high dose oral prednisone without significant improvement. One day prior to admission, patient had an outpatient biopsy of buccal mucosa performed. On presentation to the hospital, physical examination revealed diffuse oral mucositis on her lips and buccal mucosa. On hospital day two, she complained of dysuria and dry eyes. Exam was notable for genital erosions. Ophthalmologic exam showed no uveitis or episcleritis,. Laboratory evaluation for autoimmune etiologies including,human leukocyte antigen B51 and infectious workup including HSV 1/2 PCR, CMV, HIV, fungal cultures and mycoplasma serologies were all negative. CT scan of neck and chest showed prominent bilateral cervical lymphadenopathy without discrete masses. Pathology results from the initial biopsy were suspicious for p16 negative invasive squamous cell carcinoma (SCC). On hospital day 7, she developed a 1-cm ulcerative lesion on her left jaw. Punch biopsy of the new jaw ulcer was performed. Pathology with immunofluorescence and immunobullous panel revealed a final diagnosis of pemphigus vulgaris (PV). Following discharge, she was started on high dose prednisone (80mg daily), intravenous immunoglobulin, and rituximab.
Discussion: This case demonstrates the diagnostic challenges of PV which can present without classic findings and can clinically mimic other conditions including infection, neoplasm, drug reactions, and other autoimmune conditions. Dental work may trigger onset of symptoms. Patients may present with mucosal lesions prior to the development of other skin findings With mucosal involvement, frank vesicles and bullae often are not seen. In this case, initial pathology findings concerning for SCC and the recent positive HSV-1 PCR led to a delay in diagnosis and treatment.
Conclusions: This case reinforces the importance of avoiding cognitive biases like anchoring based on prior history and preliminary pathology findings. Biopsy with immunofluorescence is the gold standard for diagnosis of PV and should be completed as early as possible, as routine pathology may be misleading. Early recognition and rapid initiation of immunosuppressive therapy can prevent complications including severe odynophagia and resulting malnutrition.
.png)