Background: Medicine is complex with extraneous workload impacting the daily flow of physicians. This may contribute to an increased risk of burnout (BO). Cognitive load from complex systems can decrease performance and increase risk of error. This study aims to evaluate the physician cognitive load (PCL) of a clinical workday in a national sample of U.S. physicians using the NASA-task load index (NASA-TLX) and evaluate its relationship with BO.
Methods: A national survey of U.S. physicians surveyed during October 2017 to March 2018. Among the responding physicians in active practice, 4622 of 5276 (87.6%) completed at least one question of the NASA-TLX. The outcome of interest, BO, was measured using the emotional exhaustion (EE) and depersonalization (DP) scales of the Maslach BO Inventory (MBI). The six sub-subscales of the NASA-TLX are: mental, physical, temporal demands, performance, effort, and frustration (ranging 0-100, 100 the highest level of demand). The sum of these six domains was determined to evaluate the PCL burden of a clinical work day. Multivariable logistic regression was used to assess the relationship between BO (DP and EE as dichotomous variable) and quintiles of PCL (as well as a separate continuous model of PCL) adjusted for age, gender, hours worked per week, practice setting and specialty.
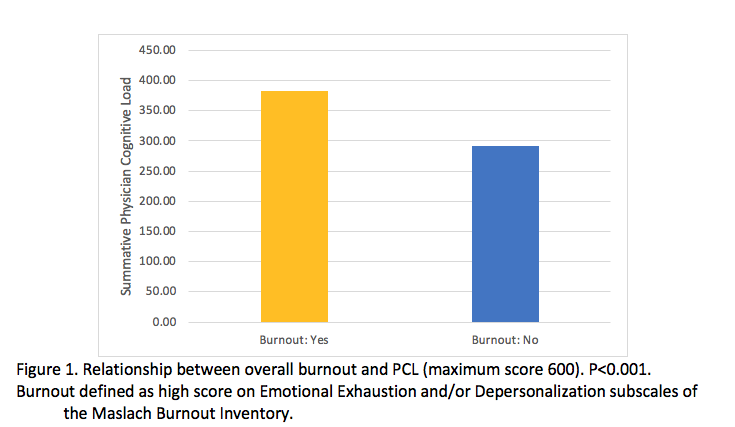
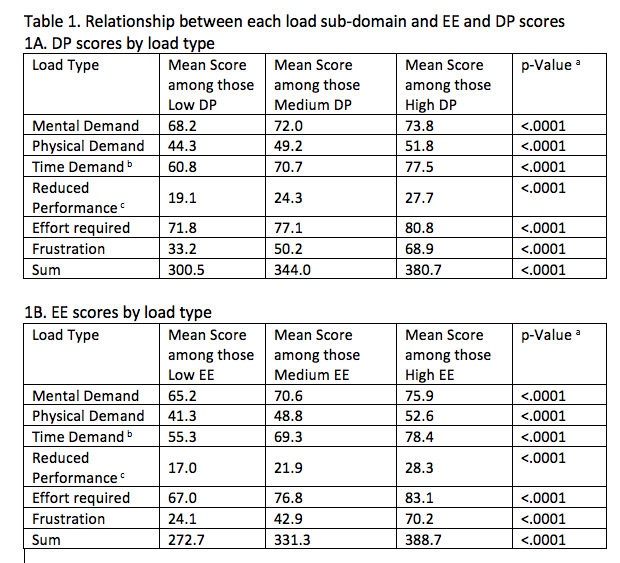
Results: A variation in mean PCL score was seen ranging 287.4 in Psychiatry to 369.8 in Emergency Medicine. PCL was strongly correlated with EE and DP scores and the risk of BO (Figure 1, Table 1).
Multi-variable analysis adjusting for age, gender, specialty, weekly work hours, and practice setting showed risk of BO increased as PCL score increased. Relative to the lowest quintile for PCL score, the OR for BO increased in a step-wise manner (2nd quintile OR=2.088 [95% CI 1.63 to 2.68]5, 3rd quintile OR= 4.43 [95% CI 3.78 to 5.65], 4th quintile OR=9.84 [95% CI 7.65 to 12.64], 5th quintile 28.6 [95% CI:21.69- 37.9]). For every 30 point (5%) decrease in average the PCL score there was 35% lower odds of experiencing BO (OR: 0.65, 95% CI: 0.63- 0.67, P= <.0001).
Conclusions: This is the first national study to evaluate the PCL associated with the daily clinical work of US physicians. Though PCL varied by specialty and setting, we found that it was strongly associated with the risk of BO independent of age, gender, practice setting, specialty and hours worked per week. These observations suggest utility of testing interventions designed to reduce PCL or mitigate risk of burnout when high PCL is unavoidable.